Achilles Tendinitis
Achilles Tendinitis
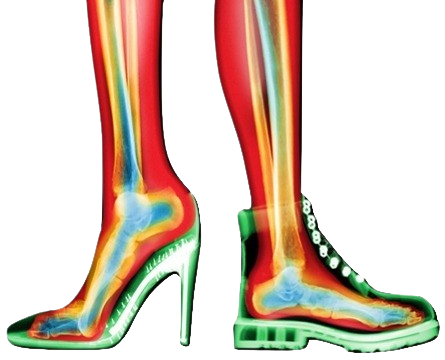
Achilles Tendinitis describes damage to your Achilles tendon in the area where it attaches to the back of the heel bone. This results in discomfort, pain, and a strain at the back of the heel which can shoot up the back of the leg.
It is often referred to as Achilles Tendinopathy and Achilles Tendinosis.

Anatomy
The Achilles tendon is a thick, fibrous band and the thickest tendon in the body. It attaches the calf muscles (gastrocnemius and soleus, plus the plantaris muscle) at the back of your leg to the back of the heel bone (calcaneus).
What causes Achilles Tendinopathy?
Large amounts of force/strain on the tendon overload it, causing the tendon fibers to become damaged and sustain micro-tears. At its worst, partial tears or even complete ruptures may result.
Many activities can strain the Achilles tendon as the tendon is used for every step we take. Common causes include:
- Increasing training intensity
- Increasing hill running duration
- Unsupportive footwear with low-set heels
- Tight calf muscles
- Bony prominence at the back of the heel
- Abnormal foot biomechanics that exacerbate the pull on the calves and Achilles
- Having pronated or high-arched feet
- Running/jumping sports such as basketball
One of the greatest causes of developing this tendonitis is ignoring early Achilles pain and continuing to exercise in the hopes that it will resolve. When pain occurs in the Achilles tendon, it’s important that you stop the activity causing the pain.
What are the symptoms?
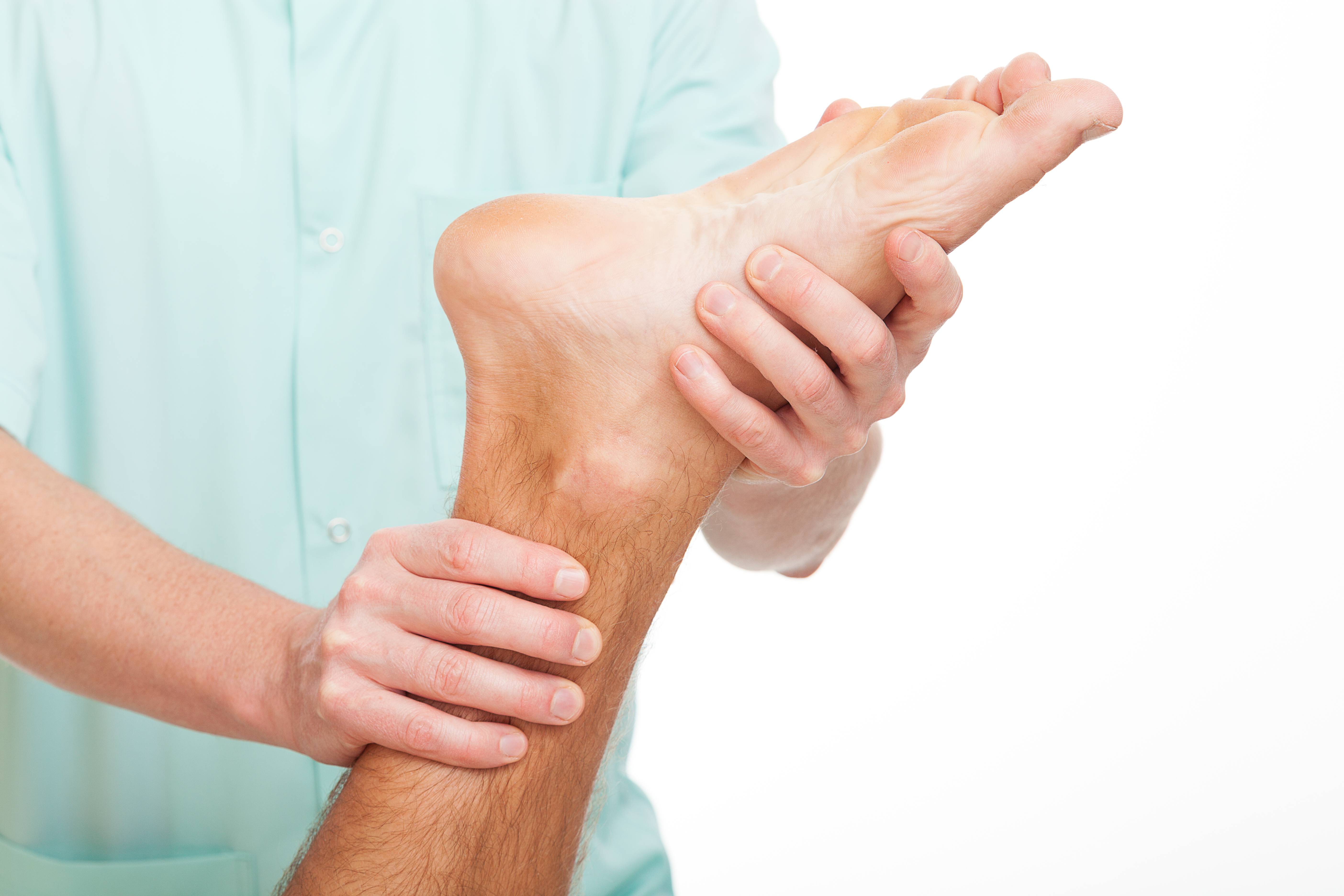
Generally, symptoms involve pain and tenderness through the Achilles tendon, whether it be at the insertion at the heel or further up the tendon at the back of the heel. Pain ranges from mild discomfort to severe pain. Symptoms include:
- Pain that is exacerbated by running, especially uphill
- Pain on pinching the Achilles tendon
- Stiffness through the back of the heel and up the leg, especially in the morning
- Inflammation of tissues surrounding the Achilles tendon
- Pain on rising onto the toes
Treatment
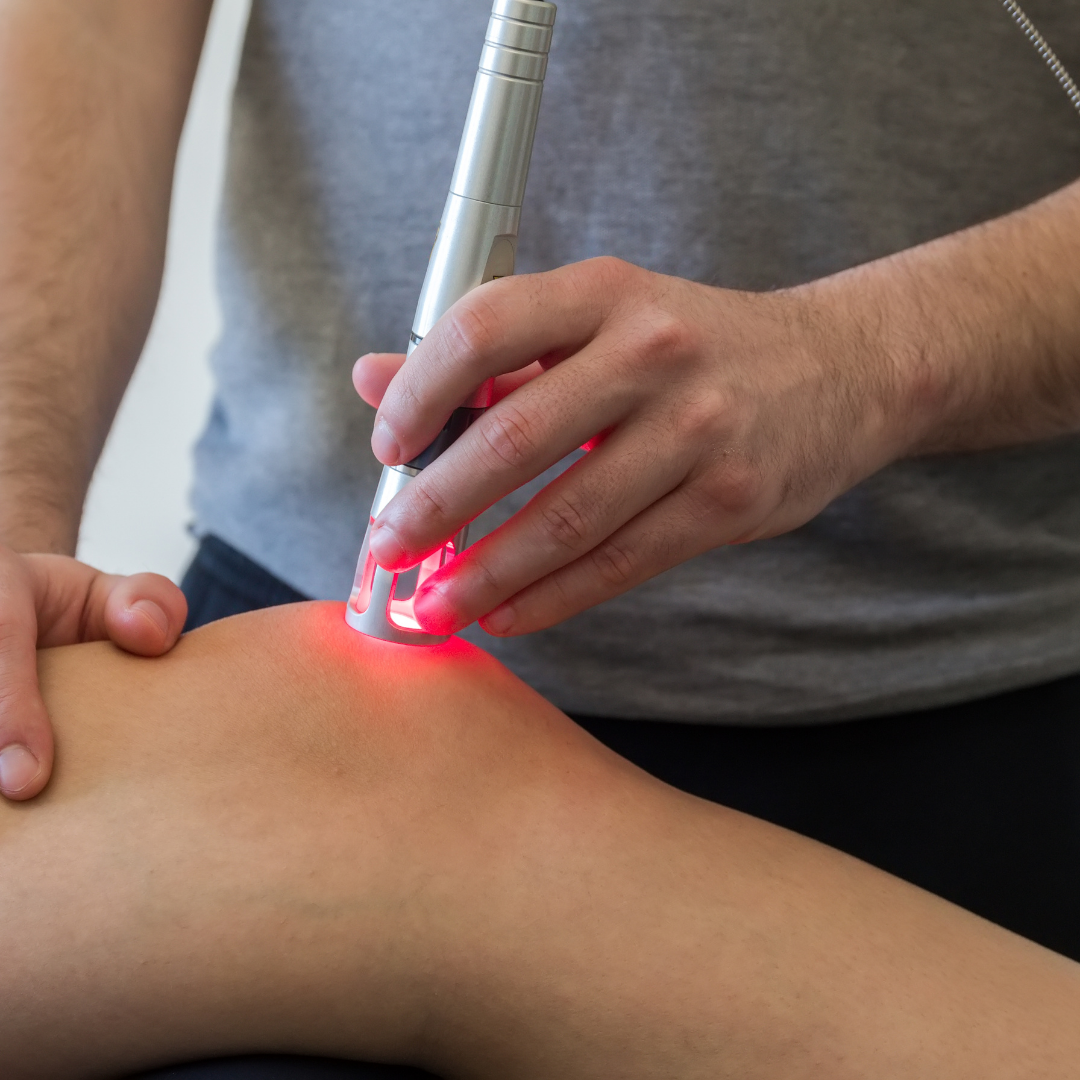
The first step is to manage the initial painful symptoms using RICE (rest, ice, compression, and elevation). It’s important to refrain from the activity that initially triggered the pain so that it doesn’t worsen and become more difficult to manage. From there, we’ll discuss the most appropriate treatment plan for you based on your current symptoms and history. These may include:
- Footwear – More supportive and cushioned footwear during and after your treatment
- Orthotics – correcting any biomechanical abnormalities and alignment issues that may be contributing to your pain and problems
- Heel lifts – to reduce strain on the Achilles tendon
- Stretching – stretching any tight muscles that may be pulling on the Achilles tendon and contributing to the pain
- Strengthening – when appropriate, restoring strength to the weakened tendon to restore full functional capacity
You can read more in this blog about Achilles Tendinopathy.
Terminology
While the following terms are often used interchangeably to describe pain at the back of the heel from the Achilles tendon, Achilles Tendinopathy, and Tendinosis describe degenerative changes to the tendon. This means the weakening of the tendon over time, even after inflammation has settled. Tendinitis denotes an inflammatory response (‘itis’) following damage and irritation.
Often in an injury, there is an initial inflammatory response, but after it settles and without adequate care, the degeneration continues to progress. Continued non-inflammatory degeneration following an injury is most commonly referred to as Tendinosis. Tendinopathy is more of a general term for tendon degeneration, without specifying the nature of the cause.
Because the Achilles tendon has a poor blood supply along the length of the tendon and a good blood supply is essential for effective healing and repair, this means that there is a tendency for the tendon to progress into a degenerative state as opposed to staying ‘inflamed.’