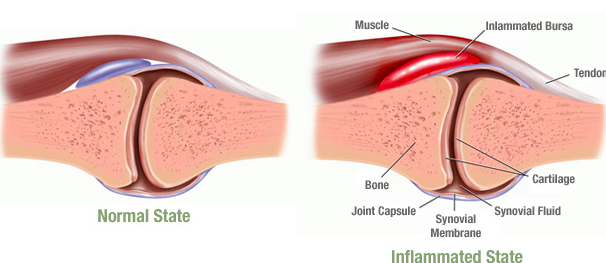
Bursitis describes the inflammation of a bursa, a small fluid-filled sac that sits between two structures in our bodies, often tendon and bone. A bursa works to reduce friction between its surrounding structures, lubricating them so they glide smoothly past one another, instead of rubbing against one another and causing damage. We have over 150 bursae throughout our body and the term ‘bursitis’ is often associated with the location of the particular affected bursa, for example, retrocalcaneal bursitis.
Bursitis typically results from repeated irritation to a particular bursa, such as overuse or excess pressure through from strenuous activity with high loads. This may be contributed to by poor biomechanics and function of the lower limbs. The irritation causes swelling and the onset of painful symptoms. Trauma/injury in the region of the bursa can also cause bursitis, as well as certain systemic inflammatory conditions, such as rheumatoid arthritis or gout. Any mechanism of action that causes a bursa to become inflamed will cause pain and tenderness at the bursa itself, as well as at the surrounding structures. This is due to the extra pressure on the tendons and muscles created by the swelling of the bursa that can then begin to irritate them. Bursitis is more common as we grow older and if our work involves repetitive movements.
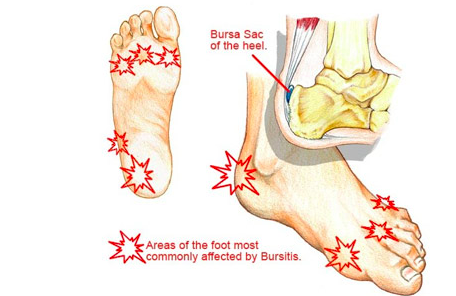
The symptoms of bursitis can include:
In the lower limbs, the most common sites for bursitis include:
Initially, the use of rest, ice and anti-inflammatories may be used to reduce the painful symptoms and swelling. Any activity that further irritates the region should be reduced as much as possible to allow the inflammation to settle and repair to occur. However, the treatment must focus on addressing the cause of the bursitis, particularly where it is a biomechanical cause, as otherwise, the symptoms are likely to recur. This is where your podiatrist will carry out a comprehensive biomechanical examination to assess the function of your lower limbs, with a focus on structures in the area of your bursitis that could be contributing to the problem. By addressing and correcting the identified issues, the same high-pressure loads at the bursa should not occur, and the chance of your bursa becoming damaged again in this way is greatly reduced. This can involve:

If you’re unsure whether you should wear walking or running shoes when exercising, this article is for you.
We explain the differences between walking and running shoes and how to determine which one is best for your feet. When it comes to buying a new pair of shoes, most people walk into a store expecting to just “find something comfy.” Then, suddenly, you’re asked: Are you looking for
walking shoes or running shoes? And that’s where the confusion begins. Because for many people, the answer isn’t that simple.
You could walk a lot – to work, around the block, chasing after the kids, or while catching up with friends. You could have also just joined
a gym or registered for the Couch to 5km. Or you could be a walker who just wants the option to go for a run if the mood strikes. So, which
shoe do you pick?

Discover why foot health is so important as we age and how Perform Podiatry supports seniors in staying mobile, independent, and pain-free. From diabetic care to personalised treatment plans, we’re here to help keep your feet happy and healthy, every step of the way.
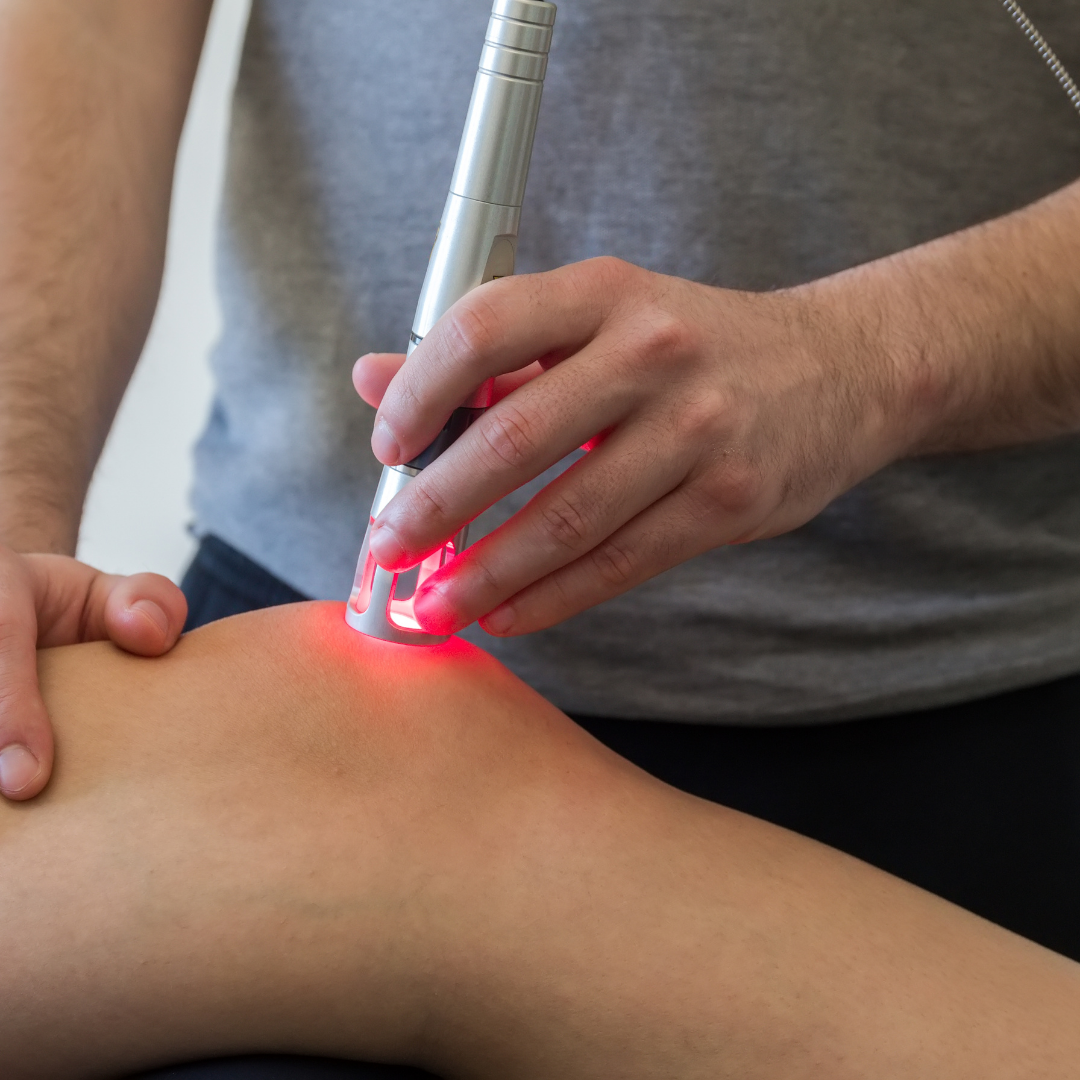
Discover how Class IV Laser Therapy at Perform Podiatry offers powerful, drug-free relief for foot and ankle pain. Backed by science, this advanced treatment helps you heal faster and move better, without the need for surgery or medication.
Keeping your family on their feet and helping them to walk, run, play and exceed their goals is why we love getting up in the morning.
Ground Floor, One Health Building
122 Remuera Rd, Remuera
Auckland 1050, New Zealand
| MON - FRI | 7:30am – 6:30pm |
| SAT | 8:30am – 4:30pm |
| SUN | Some availability |
Make an Appointment
Online Schedule
Our virtual receptionist is available 24/7 to help with general questions, booking requests, and clinic information, even when our team is busy, or it's after hours.
Whether you're calling us or using our website, you'll get fast assistance any time of day. And if your query needs a personal touch, a member of our team will follow up as soon as possible.