Rheumatoid arthritis is an autoimmune disease, as opposed to the traditional ‘wear and tear’ arthritis (osteoarthritis). It occurs when your body’s immune system attacks your own cells at the lining of the joints. This causes pain, swelling and inflammation. Rheumatoid arthritis isn’t limited to just the lower limbs but affects the whole body, primarily the small joints in the hands and feet.
 In
an RA flare, the body’s immune system attacks the joint capsule lining, called the synovial membrane. As the lining becomes
inflamed, it is no longer able to produce the synovial fluid which works to lubricate joints and nourish the cartilage and bone ends. This
means the joints stiffen and mobility becomes harder. With repetitive inflammation during flares, the cartilage and connective tissues
become damaged and the joint capsule can lose its ability to stabilise the joints. While the exact reason for the body getting
confused and attacking its own cells at the joints is not well understood, it has been thought that hereditary factors may increase
your chance of developing it. Other contributing factors include smoking and the female gender. Flares often occur without an
identifiable cause, though some causes have been attributed to stress, illness and injury. Some of those affected report that cold
temperatures and weather affect their symptoms.
In
an RA flare, the body’s immune system attacks the joint capsule lining, called the synovial membrane. As the lining becomes
inflamed, it is no longer able to produce the synovial fluid which works to lubricate joints and nourish the cartilage and bone ends. This
means the joints stiffen and mobility becomes harder. With repetitive inflammation during flares, the cartilage and connective tissues
become damaged and the joint capsule can lose its ability to stabilise the joints. While the exact reason for the body getting
confused and attacking its own cells at the joints is not well understood, it has been thought that hereditary factors may increase
your chance of developing it. Other contributing factors include smoking and the female gender. Flares often occur without an
identifiable cause, though some causes have been attributed to stress, illness and injury. Some of those affected report that cold
temperatures and weather affect their symptoms.
Rheumatoid Arthritis typically presents symmetrically. These flares come and go unpredictably and can affect many joints at once. The effects of RA progressively worsen and the joints incur more damage, until the joints are left with very little movement. This is why management has a big focus on slowing down the progression of symptoms and maintaining as much mobility as possible. Generally, symptoms include:
Your GP may be able to provide medication and other therapies to help manage the symptoms of RA and slow its progression. These will likely involve anti-inflammatory medications. As Podiatrists, we look at ways to reduce pain in the joints of your feet and legs, improving your comfort and general quality of life. Custom-prescribed orthotics are often used to increase comfort, absorb shock, and decrease the load through high-pressure areas and joints at the feet. Keeping you comfortable and mobile allows you to continue to carry out your daily activities. Exercises can also help you maintain your muscle strength and range of motion at the joints, slowing down the progression of symptoms.

If you’re unsure whether you should wear walking or running shoes when exercising, this article is for you.
We explain the differences between walking and running shoes and how to determine which one is best for your feet. When it comes to buying a new pair of shoes, most people walk into a store expecting to just “find something comfy.” Then, suddenly, you’re asked: Are you looking for
walking shoes or running shoes? And that’s where the confusion begins. Because for many people, the answer isn’t that simple.
You could walk a lot – to work, around the block, chasing after the kids, or while catching up with friends. You could have also just joined
a gym or registered for the Couch to 5km. Or you could be a walker who just wants the option to go for a run if the mood strikes. So, which
shoe do you pick?

Discover why foot health is so important as we age and how Perform Podiatry supports seniors in staying mobile, independent, and pain-free. From diabetic care to personalised treatment plans, we’re here to help keep your feet happy and healthy, every step of the way.
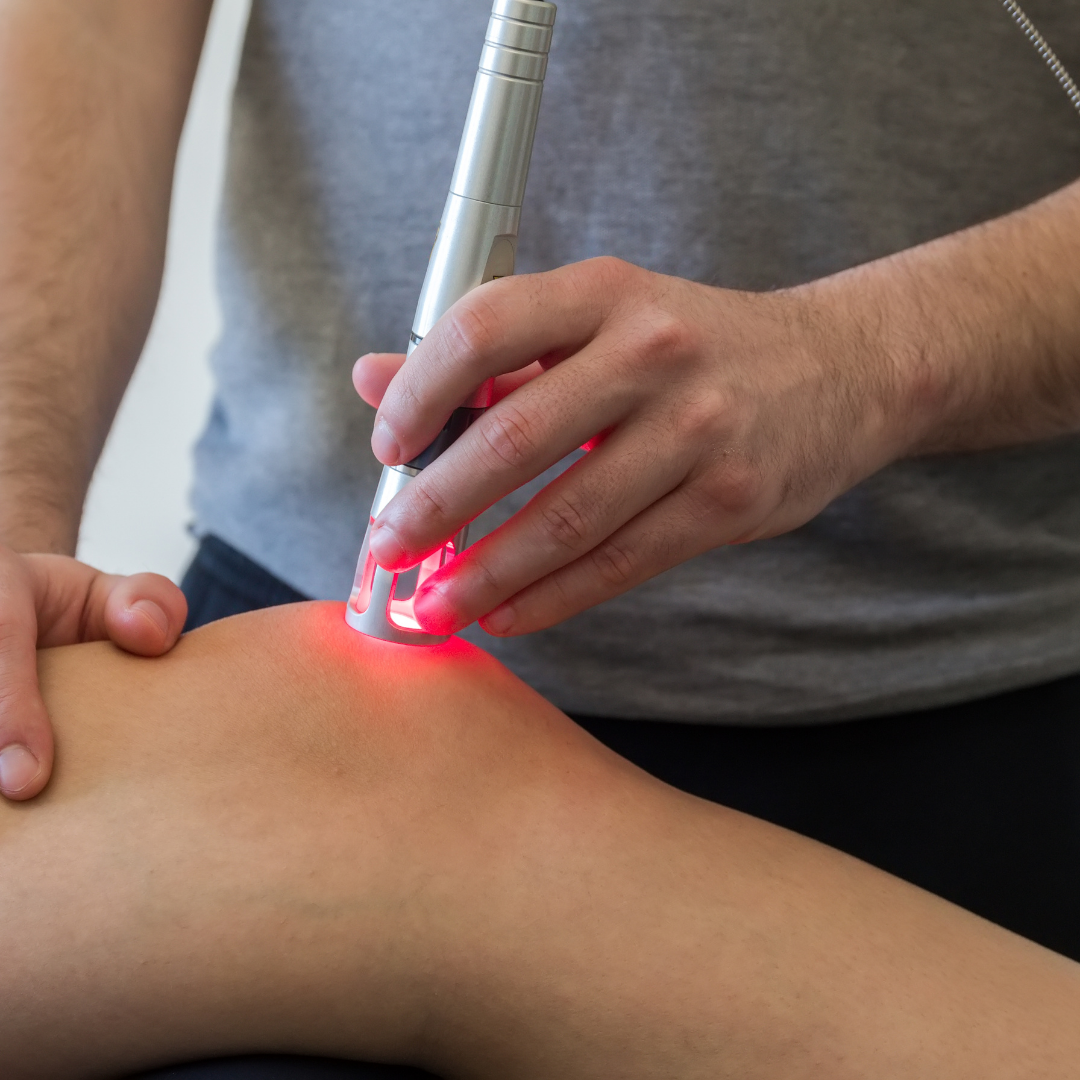
Discover how Class IV Laser Therapy at Perform Podiatry offers powerful, drug-free relief for foot and ankle pain. Backed by science, this advanced treatment helps you heal faster and move better, without the need for surgery or medication.
Keeping your family on their feet and helping them to walk, run, play and exceed their goals is why we love getting up in the morning.
Ground Floor, One Health Building
122 Remuera Rd, Remuera
Auckland 1050, New Zealand
| MON - FRI | 7:30am – 6:30pm |
| SAT | 8:30am – 4:30pm |
| SUN | Some availability |
Make an Appointment
Online Schedule
Our virtual receptionist is available 24/7 to help with general questions, booking requests, and clinic information, even when our team is busy, or it's after hours.
Whether you're calling us or using our website, you'll get fast assistance any time of day. And if your query needs a personal touch, a member of our team will follow up as soon as possible.