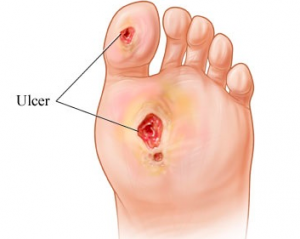
Foot ulcers are open sores on the superficial layers of the skin that result from the breakdown of healthy tissue. Ulcers may remain on the outer skin or may go as deep as to expose the underlying bone. Effective treatment for ulcers is vital as they pose a risk for serious infections, which for the lower limbs has resulted in ulcers being one of the leading causes of amputation.
Ulcers can occur due to a number of causes, both diabetic and non-diabetic. Often there is an associated medical problem or condition, so it is essential that this is uncovered and treated. Areas of high pressure over bones and joints can contribute to the development of all ulcers. They can be:
Neuropathic ulcers typically occur where the sensation is partially or wholly lost from the feet. This often happens with diabetes but other conditions can cause neuropathy too. Neuropathic ulcers can progress quickly because they are often unable to be felt and so no pain- or pressure-alleviating measures are taken. These ulcers are often located on the bottom of the foot in any area that has high pressure. Arterial ulcers result from poor circulation and blood flow to the feet and legs. Insufficient blood to the tissues can cause tissue death and the development of these often painful ulcers. These ulcers often occur on the feet and lower third of the legs. They carry a higher risk of infection as circulation is generally insufficient to help clear infections. Venous ulcers occur from problems with the veins where they struggle or fail to complete their function of moving fluid away from the legs. This leaves the fluid to pool in the legs, resulting in leg swelling, and greatly increases the venous system pressure which then leads to ulceration. These ulcers are often seen around the lower legs and ankles. Pressure-related ulcers are often referred to as pressure sores and occur from prolonged pressure to an area of the lower limbs or body. This is often observed in those confined to their beds, where ulcers develop on the buttocks or the back of the heels. Often there are other associated conditions at play too.
Foot ulcers may be circular in shape or may have distorted edges. They start as a reddened area that blister, peel or crack to create an open wound. They often weep and may have some bloody discharge. The layers of skin become thin and the ulcer may expose bone, muscle or tendon. The edges may become brown/black or stay pink/red. If an infection occurs, the ulcer may have patches of yellow/green and may produce exudate and an unpleasant odour.
Because ulcers put patients at risk of serious complications, it is important that ulcers are treated professionally and effectively. Treatment will depend on the cause of your ulcer and the contributing factors. Because of the often systemic nature of ulcers, treating the cause often involves looking at your overall circulatory issues, venous problems, and the management of diabetes where present. Your podiatrist will be able to:

If you’re unsure whether you should wear walking or running shoes when exercising, this article is for you.
We explain the differences between walking and running shoes and how to determine which one is best for your feet. When it comes to buying a new pair of shoes, most people walk into a store expecting to just “find something comfy.” Then, suddenly, you’re asked: Are you looking for
walking shoes or running shoes? And that’s where the confusion begins. Because for many people, the answer isn’t that simple.
You could walk a lot – to work, around the block, chasing after the kids, or while catching up with friends. You could have also just joined
a gym or registered for the Couch to 5km. Or you could be a walker who just wants the option to go for a run if the mood strikes. So, which
shoe do you pick?

Discover why foot health is so important as we age and how Perform Podiatry supports seniors in staying mobile, independent, and pain-free. From diabetic care to personalised treatment plans, we’re here to help keep your feet happy and healthy, every step of the way.
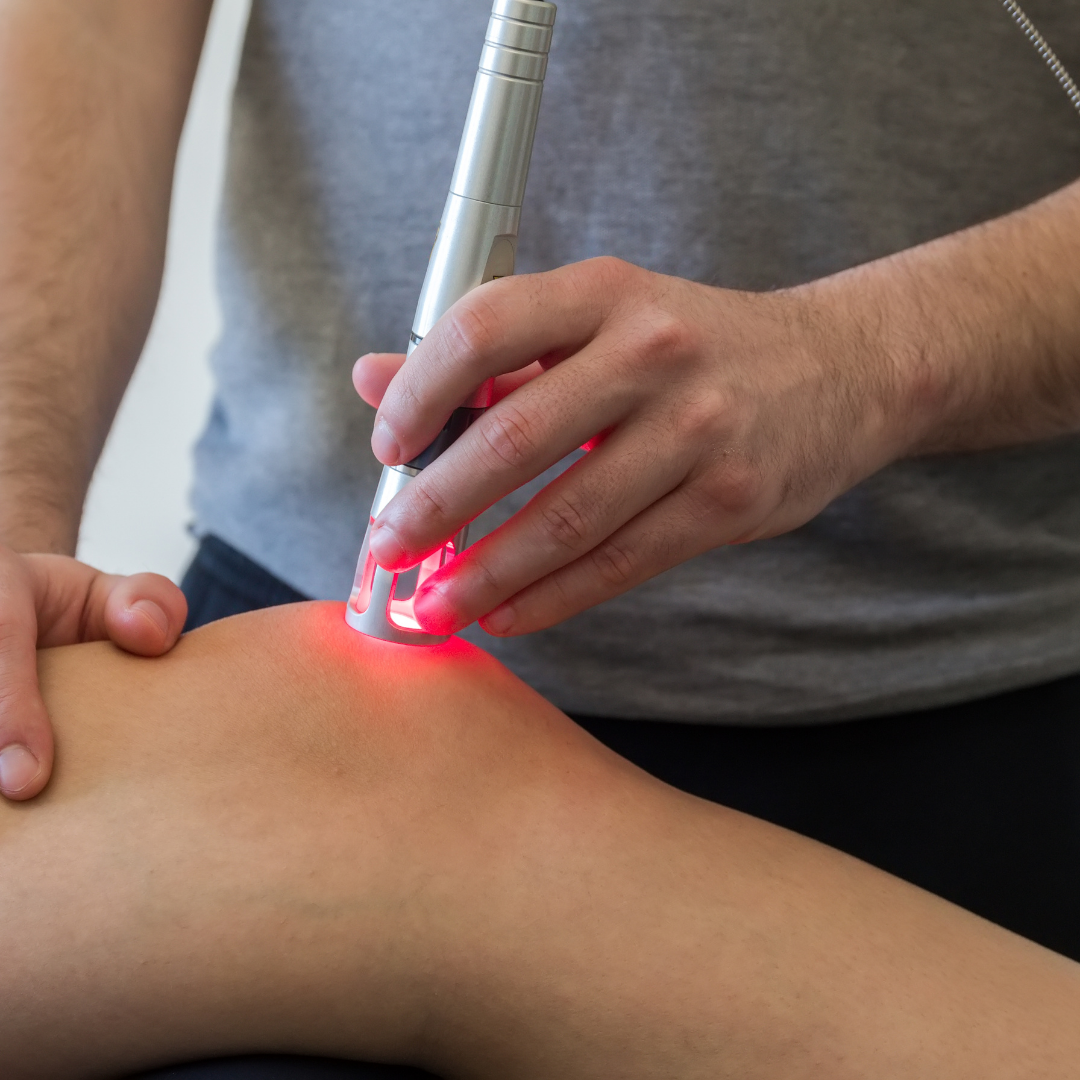
Discover how Class IV Laser Therapy at Perform Podiatry offers powerful, drug-free relief for foot and ankle pain. Backed by science, this advanced treatment helps you heal faster and move better, without the need for surgery or medication.
Keeping your family on their feet and helping them to walk, run, play and exceed their goals is why we love getting up in the morning.
Ground Floor, One Health Building
122 Remuera Rd, Remuera
Auckland 1050, New Zealand
| MON - FRI | 7:30am – 6:30pm |
| SAT | 8:30am – 4:30pm |
| SUN | Some availability |
Make an Appointment
Online Schedule
Our virtual receptionist is available 24/7 to help with general questions, booking requests, and clinic information, even when our team is busy, or it's after hours.
Whether you're calling us or using our website, you'll get fast assistance any time of day. And if your query needs a personal touch, a member of our team will follow up as soon as possible.