Athlete’s Foot describes a fungal skin infection that develops on the bottom of the feet and between the toes. It affects the outer layer of the foot and can get very itchy and frustrating. Many people will experience Athlete’s Foot at some point in their lives, or even many times, because it is easily spread through sharing surfaces with those affected. It is medically referred to as tinea pedis which literally translates to ‘ringworm of the foot’ and gets the name ‘Athlete’s Foot’ because of its high prevalence among athletes.
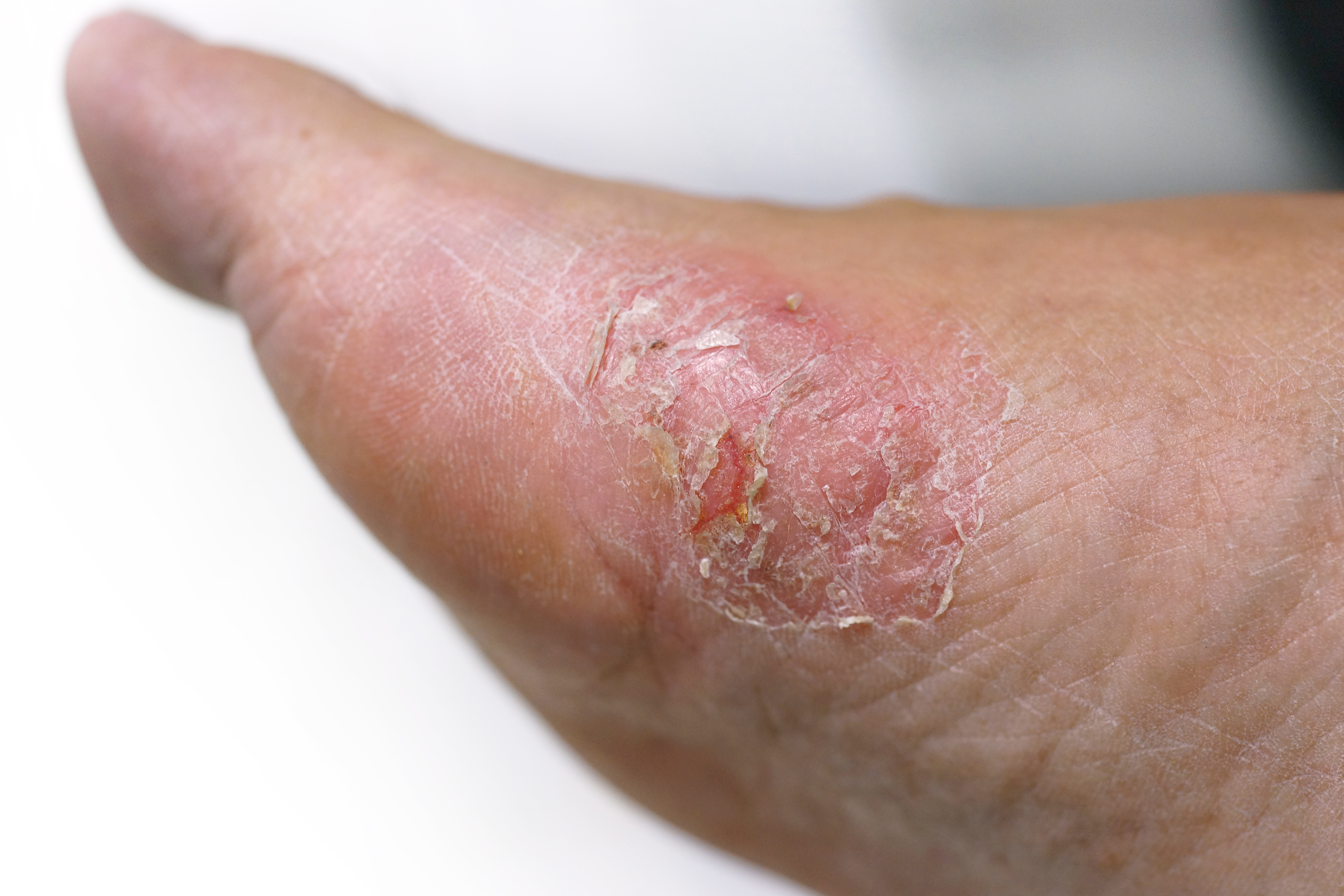 A fungus (called Trichophyton) is the cause of Athlete’s Foot and is contracted through direct contact with the fungus. When
the fungus is paired with warm and damp conditions, it can quickly grow and spread
over the bottom of the foot.
A fungus (called Trichophyton) is the cause of Athlete’s Foot and is contracted through direct contact with the fungus. When
the fungus is paired with warm and damp conditions, it can quickly grow and spread
over the bottom of the foot.
This is why the athlete’s foot is often contracted from and thrives in showers, changing rooms and closed-in shoes.
Be careful, your toenails are also vulnerable to fungal nail infections. These are often difficult to treat, even in drier and cooler conditions.
If you have contracted Athlete’s Foot, you might experience:
Before any treatment can be started, we must confirm the presence of a fungal. Your podiatrist is expertly trained to know the signs and symptoms, and can differentiate athlete’s foot from other skin conditions that may have a similar presentation. If you have the aforementioned symptoms and your feet are also particularly odorous, you may have both a fungal and bacterial infection simultaneously. If so, your required treatment will differ from a fungal infection alone. Once the athlete’s foot is confirmed, you can start by doing as much as you can at home to keep the feet dry, clean, and away from sources of infection. These typically include:
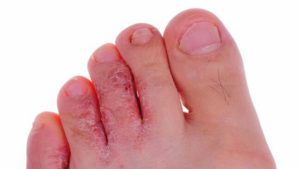
To treat the fungus directly, your Podiatrist will recommend the right anti-fungal for you to use. This may come in the form of a cream, powder, tablet or other medication. This is best decided by your Podiatrist and pharmacist as oral medications can take a toll on your liver, so must be carefully assessed with regard to your overall health. If the infection has spread to your toenails, you’ll also need to treat the nails too. This can often be significantly more difficult than treating the skin alone as the fungus can penetrate the nail bed. Your Podiatrist will advise you on the best course of action for this. To learn more about fungal nail infections, click here. Throughout your treatment, care must be taken as the infection can make your skin very fragile and susceptible to damage.
Because fungus spreads so easily, care must be taken to avoid re-infection. Re-infection doesn’t have to come from another person, but can occur from continuing to wear your own infected shoes and socks. We will explain the best ways to minimise your risk of re-infection to keep the fungus gone. This can include anything from scrubbing down your showers with appropriate anti-fungal agents to hot washing all of your socks, bath mats and shoe liners with anti-fungal washing detergent.

There’s something special about a chilling morning. The quiet air, a warm cup of coffee, and a slow start before the
day begins. But for many people, that peaceful moment is interrupted by a sharp reminder the second their feet hit the floor.

Valentine’s Day is about love, appreciation, and thoughtful gestures but let’s be honest, most gifts don’t last longer than a week. This year, choose something different. Choose a gift that offers comfort, confidence, and real care: a Medical Pedicure.
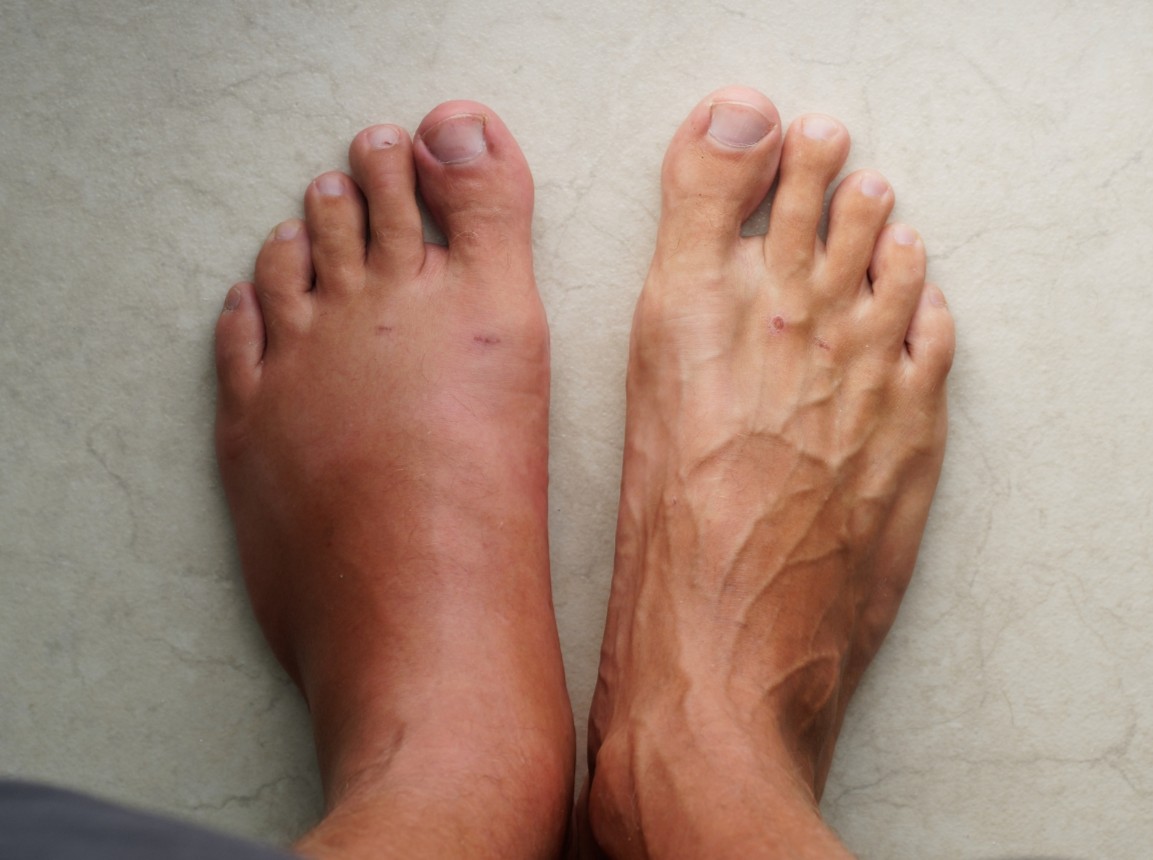
We’ve all had those days — you come home after hours on your feet, kick off your shoes, and notice your ankles look puffier than usual.
Swelling in the feet, ankles, or legs (known medically as edema) isn’t always a reason to panic. It can be as simple as a
salty lunch or a long flight.
But what if it’s happening more often — or seems to be getting worse? Swelling can sometimes be a sign of something more serious. Here’s
what could be going on and when to check in with your doctor.
Keeping your family on their feet and helping them to walk, run, play and exceed their goals is why we love getting up in the morning.
Ground Floor, One Health Building
122 Remuera Rd, Remuera
Auckland 1050, New Zealand
| MON - FRI | 7:30am – 6:30pm |
| SAT | 8:30am – 4:30pm |
| SUN | Some availability |
Make an Appointment
Online Schedule
Our virtual receptionist is available 24/7 to help with general questions, booking requests, and clinic information, even when our team is busy, or it's after hours.
Whether you're calling us or using our website, you'll get fast assistance any time of day. And if your query needs a personal touch, a member of our team will follow up as soon as possible.
If you’d like to see a podiatrist who speaks your preferred language, just give us a call and we’ll help you book.