
With winter well and truly here, we find ourselves bidding farewell to sandals and embracing cosy merino socks. However, for podiatrists like us, the arrival of winter also means an increase in patients seeking help for specific foot problems that arise due to the colder temperatures. To help, here are our valuable podiatry insights into the top five winter-specific foot problems we often encounter, along with practical tips to keep your feet safe and protected.
Raynaud’s Phenomenon
The first condition we tend to see is called “Raynaud’s phenomenon” or syndrome. Raynaud’s affects both the feet and hands, and it is triggered by cool temperatures. If you experience Raynaud’s, you’ll notice that certain parts of your feet, particularly the toes, turn stark white, resulting in patchy discolouration. Other areas may turn red or blue or purple, and you may also feel extreme coldness and numbness in your feet.
Raynaud’s occurs when the blood vessels in your feet constrict, limiting blood flow. Interestingly, stress can also contribute to the onset of Raynaud’s symptoms. As normal blood flow returns, you may experience sensations of heat, tingling, throbbing, or swelling in your feet.
What can you do? The key is to keep your feet warm and dry. When your feet are warm, the blood vessels widen, promoting circulation and preventing episodes of Raynaud’s.
Dry, Cracked Skin
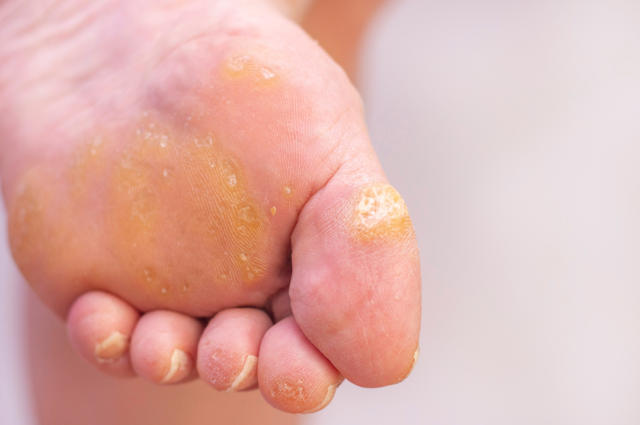
Did you know that the soles of your feet lack oil glands? This means that they are prone to drying out, especially in colder temperatures. Dry skin reduces sensitivity in our feet and makes us more susceptible to calluses and cracks, particularly on the heels.
What can you do? The solution is simple: moisturise daily. Regularly applying moisturiser is crucial since your feet cannot naturally keep the skin moist. You don’t need expensive skincare products; your regular moisturiser will suffice to keep your skin smooth, supple, and healthy. If you notice a significant callus build-up, consider having it reduced by your podiatrist. The same applies to any cracks that form in the heels.
Fungal Nail And Skin Infections
Fungus thrives in warm, moist, and dark environments—just like the conditions found in our enclosed winter shoes and warmer socks. Spending all day in these environments, combined with increased rainfall and foot sweating, creates the perfect breeding ground for fungal infections.
However, fungal infections don’t simply materialise; you must come into contact with fungal spores. Whether it’s at a friend’s house, your local gym, or a swimming pool, if you pick up the infection, there’s a higher chance it will spread faster than in summer when going barefoot or wearing sandals allows your feet to dry out.
What can you do? After every shower or when removing your shoes, thoroughly dry your feet. If your shoes get wet, let them dry completely before wearing them again, and ensure your feet are dry too. Wash and dry your socks thoroughly, paying attention to the spaces between your toes. Consider using sprays or powders on your feet or in your shoes to maintain a dry environment and discourage fungal growth. If you notice signs of a fungal nail infection (discoloration or patches on your toenails) or athlete’s foot (bubbles in the skin, dryness, itchiness, or redness), seek treatment from a podiatrist who can provide the appropriate antifungal care. The earlier you address a fungal infection, the easier it is to treat and eliminate.
Ingrown Toenails
Colder temperatures often mean thicker socks, which, combined with snug-fitting shoes, leave less room for your feet. As your toenails grow, they may press against the skin due to the restricted space, significantly increasing the risk of developing ingrown toenails.
What can you do? Keep your nails trimmed straight across the nail, avoiding cutting into the sides. If your toes feel uncomfortable and cramped in thick socks, opt for thinner socks made from warm and durable materials like merino.
Amplified Effects Of Diabetes On The Feet (Sensation And Blood Flow)
For individuals with diabetes, the impact on nerves and blood vessels gradually diminishes sensation and circulation in the feet. Colder temperatures can amplify these effects, similar to what occurs in Raynaud’s phenomenon. Consequently, it is crucial to diligently monitor your feet during this time, ensuring you don’t sustain any unnoticed cuts or wounds that could lead to infection.
What can you do? Make it a habit to check your feet daily, examining both the top and bottom. If necessary, use a mirror to inspect the bottom of your feet. Keep your feet protected and warm at all times, even indoors by wearing socks and slippers. Avoid exposing your feet to direct heat, such as open fires or hot water bottles, as decreased sensation may prevent you from feeling potential burns. Regularly moisturise your feet to maximise your sensation. Additionally, ensure you have your annual diabetic foot health check to stay informed about your foot health status and understand the specific precautions you should take.
Need Help Caring For Your Feet?
Our experienced podiatry team is here to help, and leave you feeling great on your feet. Book your appointment online here or call us on 09 523 2333
While most of the time our patients are confident about an ingrown toenail diagnosis, we thought we’d share the case of a recent patient who thought she had a very painful ingrown toenail – only to discover that she actually had a corn in the area where an ingrown toenail would normally be found.
The Symptoms
Jess* has had several ingrown toenails in the past, treated by another provider, prior to coming to see us, so she knew the symptoms she was looking out for. Aside from knowing that her work shoes that she spent 8-10 hours in per day weren’t there best for her feet and made her toes feel cramped, she also experienced:
- Pain and tenderness at one edge of her right big toenail
- Redness that was isolated to one side of the toenail
- Mild swelling around the area
- Pain when pushing down on the side of the nail from the toe
She didn’t have any bleeding or discharge, and she didn’t normally have that with her previous ingrown toenails. There were no signs of infection or indications of anything sinister. It just felt like another ingrown toenail.
Jess had always had her nails “temporarily” managed where the offending nail edge was removed, but nothing was done to stop it from coming back. She found us through our reputation of being Auckland’s leading providers of ingrown toenail treatments, including permanent solutions that would keep the ingrown toenail gone.
What Was Found
During Jess’ exam with our podiatrist, we uncovered that she didn’t actually have an ingrown toenail. The ridge that her toenail naturally followed as it grew out (on the painful side of the nail) looked like it had been rubbing against the skin (likely contributed to by her footwear) and it had actually formed a small, hard corn down the side of the nail. As corns are firm, dead skin that often blend into the appearance of the surrounding skin, Jess never even saw it until we pointed it out.
The thing with corns – and you’ll know if you’ve had one in the past – is that despite their small size, they can be incredibly painful. When present on the bottom of the foot, many of our patients describe them as constantly walking on a painful pebble. All her symptoms made sense – especially if the nail kept pressing against the corn, leading to her pain and redness.
Treatment
The best part for Jess was that her treatment was very simple and straightforward. All we had to do was use a fine surgical scalpel to remove the corn – a procedure that is painless given that corns do not have any living tissue. Once the corn was removed and the toenail was no longer pressing against anything, she felt immediate relief, and was completely pain-free by the following evening.
Did She Have Ingrown Toenails Previously?
The biggest question that was left for us is whether Jess really did have ingrown toenails in the same spot previously, or if she had had that corn for quite some time and it was misdiagnosed as an ingrown toenail given the symptoms were the same. As she previously had a small part of the nail removed to relieve her symptoms, it would make sense that once the part of the nail that would otherwise rub against the corn was removed, that her symptoms would stop too, so it would appear that her ingrown nail was ‘treated’ – without ever treating the true cause of her problem, meaning that it would be bound to continue recurring as the nail grew out.
Interestingly, that’s something that’s almost impossible to determine now – but what we do know is that Jess won’t be having any more pain related to that particular corn.
Ingrown Toenail Facts
- Aside from wearing shoes that are too tight or narrow, the biggest cause of ingrown toenails that we see and treat is a person’s nail-trimming technique – especially if they pick at or pull of the nail
- Ingrown toenails do not usually get better without treatment – a true ingrown toenail means that part of a toenail has embedded itself down in the skin of your toe (like a sharp dagger) and it must be removed
- You don’t have to suffer with repeated ingrown nails – permanent treatments that get rid of the issue once and for all are available. This involves removing a small section of the nail and then applying a chemical that destroys the nail growing cells so they don’t grow back.
- We see just as many children (often adolescents) with ingrown nails as adults. We have also successfully treated ingrown nails on young toddlers. They can occur at any age
- Having an ingrown nail where the nail has pierced your skin means that you are vulnerable to infection as long as the nail is in there and you have an open wound.
For safe and effective treatment of ingrown nails by Auckland’s leading podiatry specialists, book in at our clinic in Remuera. You can call us on 09 523 2333 or book online here.

