 Learning that you have fragile bones can be concerning, and for many, leave them with a lot of questions:
Learning that you have fragile bones can be concerning, and for many, leave them with a lot of questions:
- Why have I got fragile bones?
- What does having fragile bones mean?
- What are my risks?
- What can I be doing to improve my bone health?
With many of the patients we see and treat being diagnosed with osteoporosis or osteopenia, today our team is sharing what it means to learn that you have “fragile bones”, and how you can best protect your bone health and overall health going forwards.
What Does It Mean To Have Fragile Bones Or Poor Bone Health?
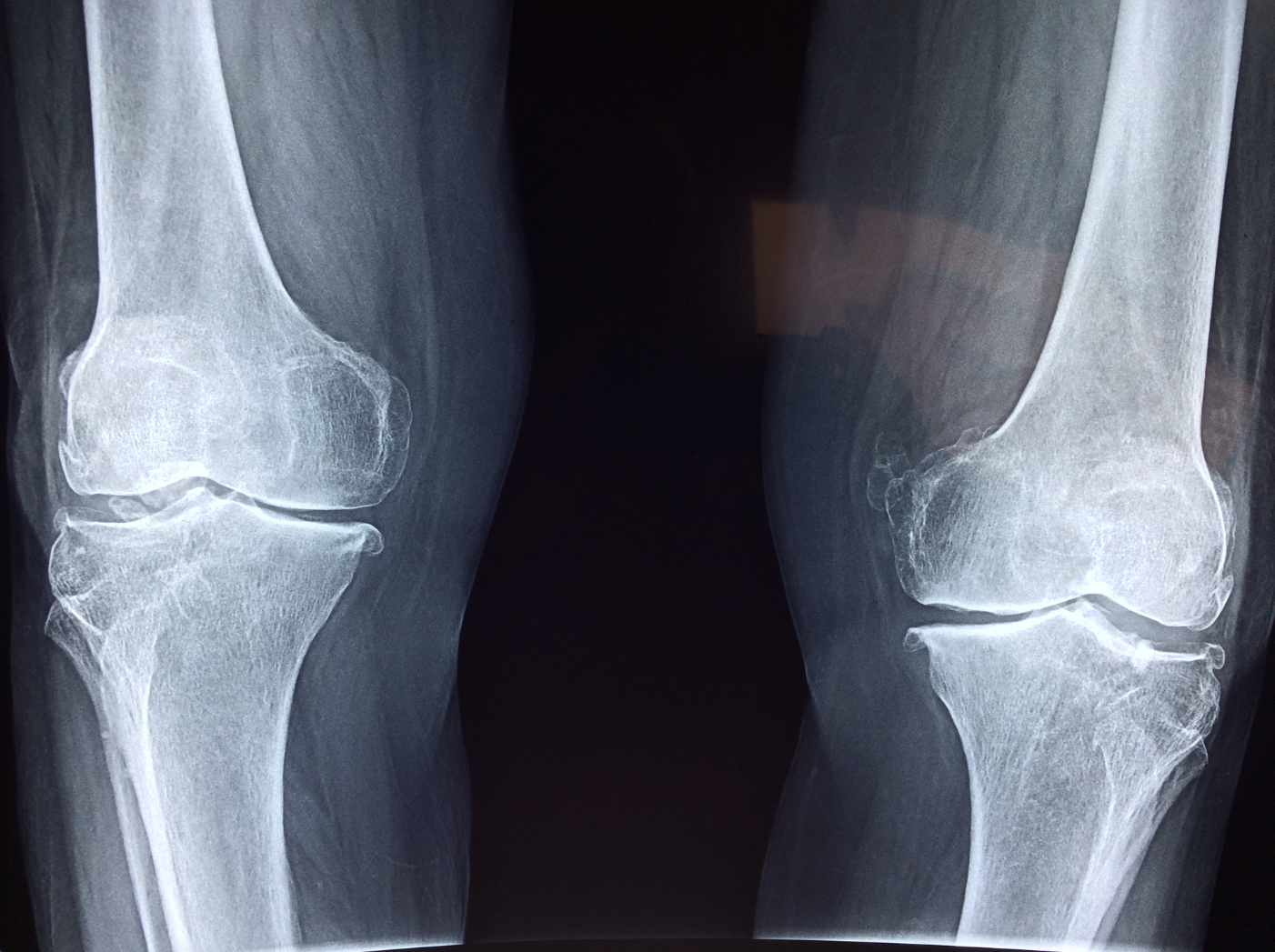
If you have fragile bones, it means that the mineral density in your bones has decreased. Clinically this can either be classed as:
- Osteoporosis: a condition that means “bones with holes”, diagnosed when your bone mineral density is significantly reduced. This makes them significantly weaker and more vulnerable to fractures.
- Osteopenia: nicknamed as ‘pre-osteoporosis’, osteopenia means that your bone mineral density has decreased below normal values, but is not yet low enough for you to be formally diagnosed with osteoporosis. Osteopenia is a big warning sign that osteoporosis is not far off if your current daily activities and attention to bone health do not improve.
The symptoms of reductions in bone mineral density and either osteoporosis or osteopenia are often difficult to spot and recognise because they are “silent”, meaning that they occur within the bones without you knowing. For many people, they only learn that they have osteoporosis when bone density testing is performed, or if they have a fracture and the cause behind their fracture is investigated.
Am I At Risk For Poor Bone Health?
Looking at osteoporosis specifically, risk factors can be classed as either modifiable, meaning you can change them, or non-modifiable, meaning that you’re stuck with these risk factors.
Modifiable risk factors for poor bone health
- Physical inactivity
- Calcium deficiency from your diet
- Long-term glucocorticoid (steroid) use
- Smoking
- Being underweight with a low BMI
- Hypogonadism
- Inadequate vitamin D intake
- High alcohol intake
- Poor nutrition
- Stress
Non-modifiable risk factors for osteoporosis
- Your gender (particularly being female)
- Entering menopause or having a hysterectomy
- Age
- Race
- Genetic characteristics
- Taking certain medications that are essential in treating other medical conditions including thyroid hormone supplements, certain diabetes medications, anti-coagulants, certain chemotherapy agents, proton pump inhibitors, certain immunosuppressants and more
- The presence of other diseases including rheumatoid arthritis, cancer, kidney disease and more
How Can I Improve My Bone Health?
The first part of this conversation must be had with your GP, as medications are often involved in helping support your bone health and the bone-strengthening process. They may also recommend using hormone-replacement therapy like estrogen, and nutritional supplements like calcium and vitamin D.
In the meantime, incorporating regular weight-bearing exercise is a good place to start in helping support your bone health at home as weight-bearing exercise is proven to be a treatment and prevention method for both postmenopausal and age-associated osteoporosis. Aim for at least 30 minutes per day, 5–7 days a week.
When patients come to us with complaints about their bone health, they are often finding walking less comfortable than it used to be and may have concerns about their stability and balance. For these patients, we may use custom foot orthotics (insoles) to help optimise their comfort, support their foot function and stability, and help restore their confidence on their feet. We pair this with a footwear review to ensure the risk of falls (and hence osteoporotic fractures) is minimised.
If foot pain or discomfort is being caused by nail or skin problems like corns, calluses, cracked heels or painful or thickened toenails, we also perform our skin and nail care for immediate relief.
Book your appointment with our podiatrists by calling us on 09 523 2333 or book online here.
 Learning that you have fragile bones can be concerning, and for many, leave them with a lot of questions:
Learning that you have fragile bones can be concerning, and for many, leave them with a lot of questions:
