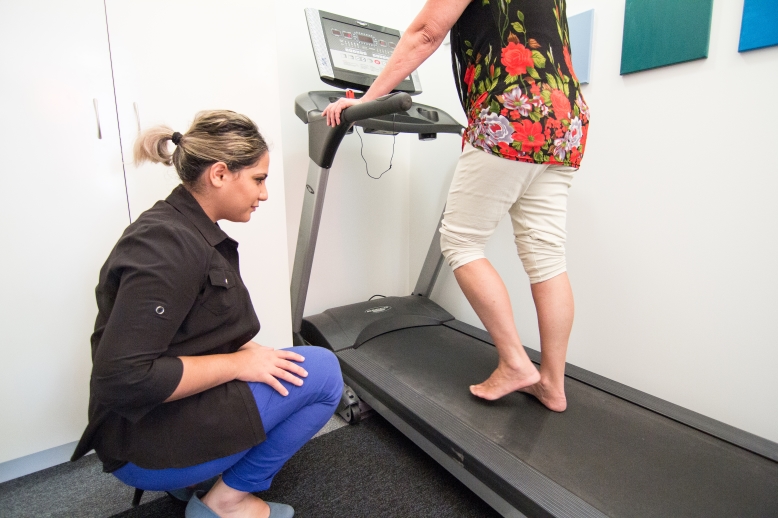
Foot and ankle pain can not only be debilitating, but also affects both our mobility and our overall quality of life. When faced with these issues, seeking the right professional expertise is crucial for accurate diagnosis, effective treatment – and getting back to feeling and moving well, as quickly as possible. In the realm of foot and ankle health, your podiatrist is your go-to foot and ankle expert. Here’s why.
Understanding The Role Of A Podiatrist
A podiatrist is a medical professional who specialises in the diagnosis, treatment, and prevention of conditions related to the feet, ankles and also the lower limbs. Their extensive training equips them to handle a broad spectrum of issues, ranging from common concerns like ingrown toenails to complex biomechanical problems influencing gait and posture including Achilles tendon pain, heel pain, shin splints, leg length differences and much more.
Why Choose A Podiatrist For Foot And Ankle Pain?
There’s a wide range of reasons that a podiatrist is the right health professional to see for your lower limb pain. These include:
They’re Experts In Foot Anatomy and Function
Podiatrists undergo extensive training focused specifically on the anatomy and function of the feet and ankles, as well as the lower limbs. Their in-depth knowledge allows for accurate diagnosis and targeted treatment plans tailored to address the unique challenges posed by this intricate area of the body.
Specialised Diagnostic Skills
Podiatrists possess specialised diagnostic skills honed through years of training and clinical experience. From identifying structural abnormalities to pinpointing the source of pain, their expertise ensures a thorough assessment of foot and ankle issues.
Comprehensive Treatment Options
Podiatrists offer a wide range of treatment options, including conservative measures, devices like braces, physical therapy, and minor surgical interventions when necessary. This comprehensive approach allows for the right, personalised care based on the nature and severity of a specific condition.
Management Of Chronic Conditions As Well As Acute Injuries
Chronic conditions such as arthritis, diabetes-related foot complications, and neuropathy require ongoing management. Podiatrists are well-equipped to provide continuous care, helping patients navigate the challenges associated with these persistent issues.
Biomechanical Expertise
Many cases of foot and ankle pain stem from biomechanical issues affecting gait and posture. Podiatrists specialise in assessing and addressing these concerns, utilising orthotics, exercises, and other interventions to restore proper biomechanical function.
Preventative Care
Beyond treating existing issues, podiatrists emphasise preventive care. Regular check-ups with a podiatrist can identify potential problems early on, allowing for proactive measures to prevent the development or progression of foot and ankle conditions.
Evidence-Based Practice
Podiatric medicine is grounded in evidence-based practice, with treatment approaches informed by the latest research and clinical guidelines. This commitment to evidence ensures that patients receive care based on proven methods and advancements in the field.
Podiatrists vs Physiotherapists
While physiotherapists play a crucial role in rehabilitation and overall musculoskeletal health, the specialised focus of podiatrists on the feet and ankles sets them apart in the context of foot and ankle pain.
Specifically, physiotherapists tend to have a broader focus on the entire musculoskeletal system, addressing issues related to muscles, joints, and movement patterns. Podiatrists, on the other hand, concentrate specifically on the lower extremities, making them more specialised in the intricacies of foot and ankle conditions. This enables podiatrists to provide more targeted interventions for foot and ankle pain, leveraging their focused skillset to address conditions ranging from toenail problems to complex biomechanical issues.
Podiatrists are also trained in both conservative and surgical interventions for foot and ankle conditions, where physiotherapists are not, being unable to perform procedures like permanent ingrown toenail correction surgery. This means that in cases where surgery is required, podiatrists can seamlessly transition from diagnosis to treatment.
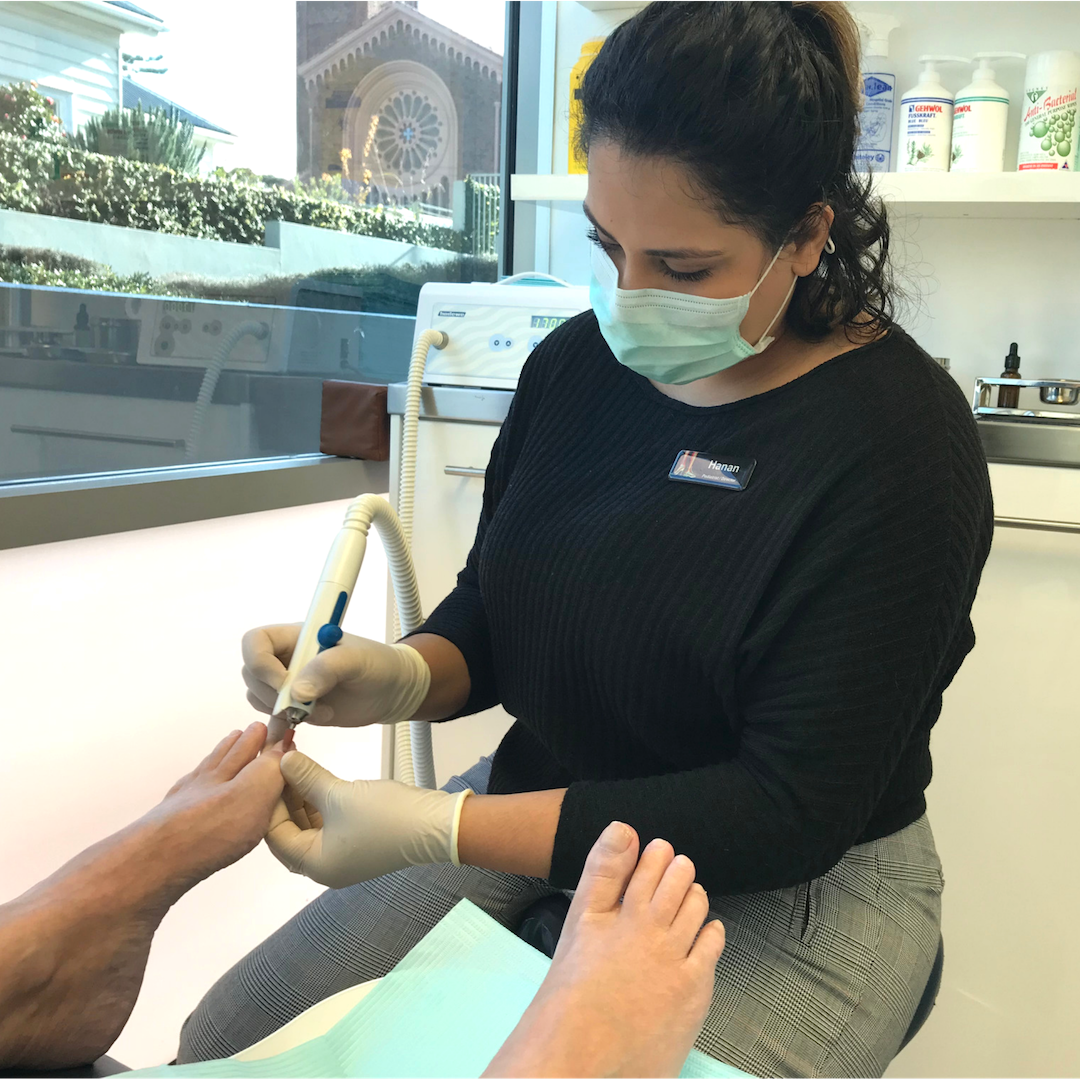


 While medical pedicures are a favourite with our patients, there are more ways that we work with our patients to help them on the slopes, including:
While medical pedicures are a favourite with our patients, there are more ways that we work with our patients to help them on the slopes, including: