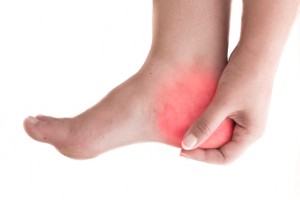
Is your child’s foot pain from a tarsal coalition?
March 25, 2018
From talking to patients about tarsal coalition, we’ve come to realise that this is a term that is not very well known by the general public, unless you or a family member has been affected by heel pain from it. Despite this, tarsal coalition does affect a number of people seeking podiatric help for heel pain, and it’s estimated prevalence around the world seems to range from less than 1% up to 2%, which in the bigger picture definitely does have a clinical significance.
This being said, we thought we’d illustrate the typical presentation of a patient with a tarsal coalition and their symptoms, so you know what to look out for in the future.
 On our end, we conduct a comprehensive biomechanical assessment in which we:
On our end, we conduct a comprehensive biomechanical assessment in which we:
Tarsal coalition: The background
For your reference, a tarsal coalition describes an abnormal connection or fusion between two or more tarsal bones of the foot. These fusions may be bony, cartilaginous or with fibrous tissue. These tarsal bones are located from the heel bone and toward the middle of the foot. The bones and joints most often affected are the calcaneus and the navicular (calcaneonavicular joint) and the talus and the calcaneus (talocalcaneal joint). One or both feet can be affected. A tarsal coalition typically occurs in the womb, leading to improper bone formation, and so is present a birth. This being said, the symptoms don’t usually start until the ages of 8+ as this is the time that bones start to mature and harden. Not all tarsal coalitions will have painful symptoms.A young patient presents
Tarsal coalition is typically diagnosed between the ages of 8 and 16 years old, and in our experience we see kids around 10-12 years old come in with their parents in the clinic. The level of activity that these kids partake in varies, though it’s often on the higher end. The pain experienced can present both as a dull ache or a sharp pain (or both) and is in the area of the affected joint, which will often be around the ankle. The pain can come and go over time, and is usually associated with physical activity. Often the pain has been left for some time (weeks ormonths) to resolve on its own, and we see the patient after it has failed to resolve for some time. Though this is our experience, we do highly recommend bringing kids in as soon as possible! The pain can stop kids from doing the things they love and participating in sports matches, as well as general daily activities as the symptoms progress. Pain can radiate to the knees and other joints, and the joints can feel stiffer, particularly around the ankle.Our assessment
 On our end, we conduct a comprehensive biomechanical assessment in which we:
On our end, we conduct a comprehensive biomechanical assessment in which we:
- Palpate around the heels and painful structures
- Check the range of motion at all the joints of the foot, ankle, knee and hip
- Conduct a gait (walking) assessment with shoes and without, on the ground and the treadmill
- Conduct a foot posture assessment
- Conduct a footwear assessment
- Check muscle strength
