
It’s
2018, and for many of us, one of our resolutions is to finally
lose that extra bit of weight. If this sounds like you, don’t worry – you’re not alone! Currently,
1 in 3 adults aged 15 years and over in New Zealand are classified as
obese, with a further
34% of adults
overweight, according to the NZ Health Survey 2017.
You may have the right workout gear ready, signed up to the gym, but what about your feet? They’re the ones that will carry you through all your workouts, runs, pump and aerobics classes. Any injuries or pains will see a halt in your progress – and a big dent in your motivation and positive attitude. This being said, if there’s one thing we can recommend to see you succeed and reach your goals, it’s this:
Get your feet and legs assessed by a Podiatrist.
We call this a
biomechanical assessment. We look at everything from:
- Your foot posture
- The way you walk (gait)
- Your muscle strength
- The range of motion available through your joints, and importantly any limitations that may be hindering you or causing you pain
- Areas of high pressure that we can redistribute to keep you comfortable and out of pain
- Muscles and tendons that are being overused and causing you to tire faster
- Your footwear
Having this assessment and being fully informed of exactly what’s happening with your feet and legs means that:
1. Your risk of previous injuries and pains returning will be reduced
We identify what is currently happening with your feet and legs in combination with any past injuries or pains that may have stopped you from reaching your exercise goals. This allows us to see why those previous injuries occurred, and therefore take precautions to ensure that they don’t happen again. This could be through changing your foot function with orthotics, strengthening certain weaker muscle groups, stretching tight muscles and much more.
2. The likelihood of new injuries developing will be reduced
Similarly to the above, we identify areas where you are at risk of developing issues and talk you through these. Perhaps you are rolling on your big toe with every step you take for much longer and with much more pressure than is normal. Short-term that might be okay, but long-term there’s a chance that area can get injured from overloading, where the bones/joints/tissues can no longer handle the large pressure. Perhaps one of your muscles is being overused with every step you take because of flat feet, resulting in your feet and legs tiring much faster than they otherwise would. Or perhaps your feet are lacking some shock absorbing qualities, contributing to generalised aching at the end of the day which can significantly worsen once you start your exercise routine.
Whatever it is, we’ll talk you through your assessment and our findings to find the best solution for your feet to keep you healthy, happy and active.
3. You can get the best shoes for your foot type
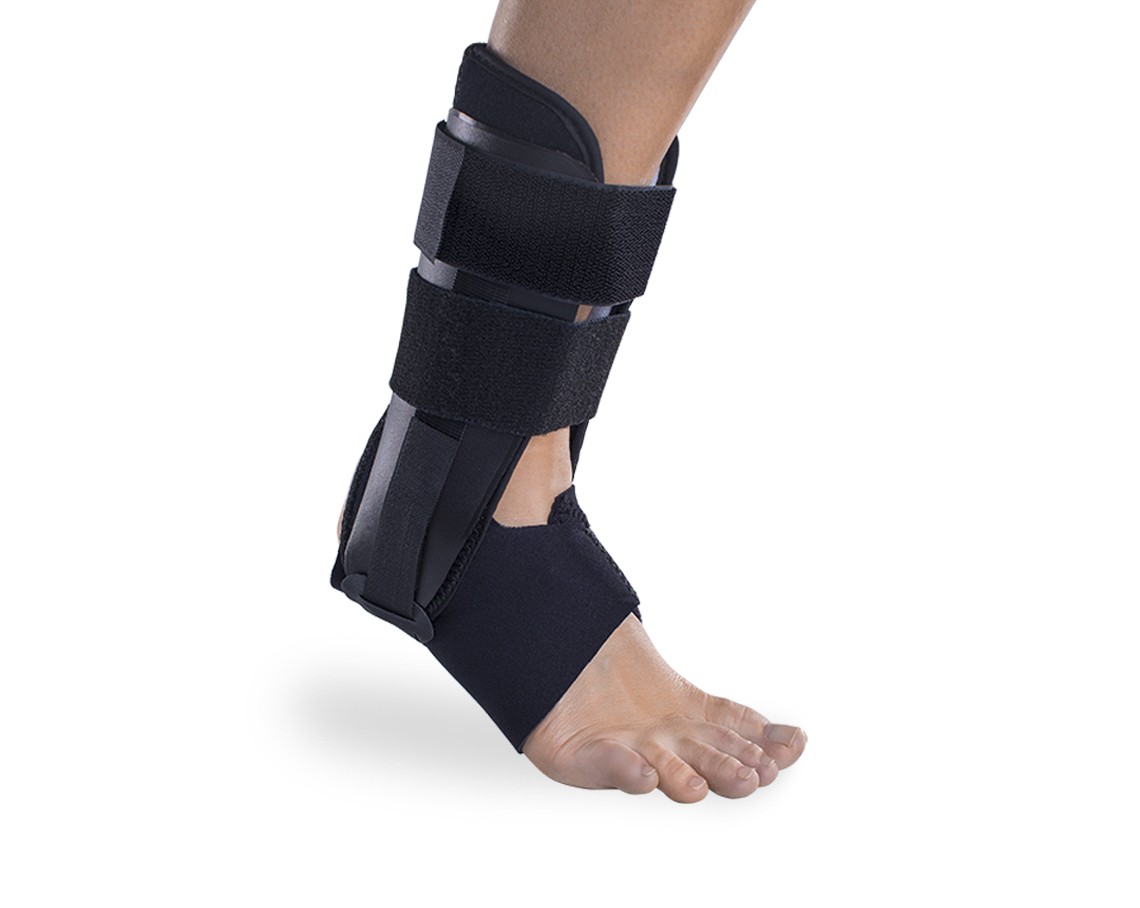
If you’ve wondered about the legitimacy of having certain shoes for your particular foot type, it’s very much true! Shoes will have different features and can either help, or sometimes hinder, your feet. A common example we see is those that have high arches and are prone to rolling their feet out (and unfortunately spraining their ankles). Because a large majority of popular shoes are aimed at flatter (pronated) feet that have more support in the arch, these can actually tip you out and further risk you injuring your ankle. We’ll give you the low-down on your feet, foot type and what shoes are best for you!
By reducing your likelihood for injury and knowing how to best take care of your feet while you’re exercising, you’re preparing yourself for the best chance of success and trust us – the preparation pays off when you can keep going and going injury-free! It’s just like the quote by Abraham Lincoln:
“Give me six hours to chop down a tree,
and I will spend the first four sharpening the axe”.
Our team at Perform Podiatry are
experts when it comes to sports medicine, the biomechanics of the feet and legs and getting you back on your feet from injury as quickly as possible! Give our friendly team a call on
09 523 2333 and start the journey to feeling great and reaching your exercise goals!
 While medical pedicures are a favourite with our patients, there are more ways that we work with our patients to help them on the slopes, including:
While medical pedicures are a favourite with our patients, there are more ways that we work with our patients to help them on the slopes, including:


 A lot of us have heard that it’s not uncommon to have a slight difference in the size of our feet or even legs. We often advise patients to buy shoes to the size of the larger foot so that toes don’t get cramped and cause pain. But when it comes to having a slight difference in the length of the legs, does it make any difference or have any effect on the body? Let’s start with the basics about limb length discrepancies.
A lot of us have heard that it’s not uncommon to have a slight difference in the size of our feet or even legs. We often advise patients to buy shoes to the size of the larger foot so that toes don’t get cramped and cause pain. But when it comes to having a slight difference in the length of the legs, does it make any difference or have any effect on the body? Let’s start with the basics about limb length discrepancies.
 It’s 2018, and for many of us, one of our resolutions is to finally lose that extra bit of weight. If this sounds like you, don’t worry – you’re not alone! Currently, 1 in 3 adults aged 15 years and over in New Zealand are classified as obese, with a further 34% of adults overweight, according to the NZ Health Survey 2017.
You may have the right workout gear ready, signed up to the gym, but what about your feet? They’re the ones that will carry you through all your workouts, runs, pump and aerobics classes. Any injuries or pains will see a halt in your progress – and a big dent in your motivation and positive attitude. This being said, if there’s one thing we can recommend to see you succeed and reach your goals, it’s this:
It’s 2018, and for many of us, one of our resolutions is to finally lose that extra bit of weight. If this sounds like you, don’t worry – you’re not alone! Currently, 1 in 3 adults aged 15 years and over in New Zealand are classified as obese, with a further 34% of adults overweight, according to the NZ Health Survey 2017.
You may have the right workout gear ready, signed up to the gym, but what about your feet? They’re the ones that will carry you through all your workouts, runs, pump and aerobics classes. Any injuries or pains will see a halt in your progress – and a big dent in your motivation and positive attitude. This being said, if there’s one thing we can recommend to see you succeed and reach your goals, it’s this:
 If you’ve ever suffered with pain at the back of your heel from your achilles tendon, you’ll know that it’s not only uncomfortable and painful but can also be very limiting to daily activities because of the massive role your achilles tendon plays in taking each step and the large amount of force it takes through every step.
What you may not know,is the importance of getting any issues or pains with your achilles tendon seen to quickly and effectively – more so than other muscles and tendons of the feet and legs. This is because unlike damage to other tendons that follows a process of swelling and inflammation, achilles tendinopathy follows a more degenerative pathway where the tendon fibres will degenerate and weaken over time.
This means that unlike other conditions where you just need to reduce the swelling and wait for it to heal, with achilles tendinopathy you actually need to actively work to strengthen the tendon as part of your rehabilitation. It also means that the longer the injury is left unmanaged, the worse it’ll get, and the more recovery time and rehabilitation it’ll require. So don’t put it off!
If you’re unfamiliar with achilles injuries, here’s a little recap on achilles tendinopathy:
If you’ve ever suffered with pain at the back of your heel from your achilles tendon, you’ll know that it’s not only uncomfortable and painful but can also be very limiting to daily activities because of the massive role your achilles tendon plays in taking each step and the large amount of force it takes through every step.
What you may not know,is the importance of getting any issues or pains with your achilles tendon seen to quickly and effectively – more so than other muscles and tendons of the feet and legs. This is because unlike damage to other tendons that follows a process of swelling and inflammation, achilles tendinopathy follows a more degenerative pathway where the tendon fibres will degenerate and weaken over time.
This means that unlike other conditions where you just need to reduce the swelling and wait for it to heal, with achilles tendinopathy you actually need to actively work to strengthen the tendon as part of your rehabilitation. It also means that the longer the injury is left unmanaged, the worse it’ll get, and the more recovery time and rehabilitation it’ll require. So don’t put it off!
If you’re unfamiliar with achilles injuries, here’s a little recap on achilles tendinopathy:
 Activities that put a lot of force and strain through the tendon. This includes:
Activities that put a lot of force and strain through the tendon. This includes:
 Does it feel like you’ve been walking around on an uncomfortable small stone beneath your foot for some time now? Have you been feeling pain at the forefoot that seems unusual? And that while Google tells you this pain should be located beneath the big toe joint or at one of the other toes along the ball of your foot, you’re actually feeling it up from there, through the long bones of the foot? Perhaps around your 3rd and 4th long toe bones? And maybe instead of the usual pain, redness and swelling, the pain and discomfort comes with a twinge every so often that may tingle or feel numb?
If this sounds familiar then you, my friend, may have a Morton’s Neuroma.
What is a Morton’s Neuroma?
A neuroma describes a thickened or inflamed nerve in a space between the toes (interdigital space). Just like rubbing and irritating a muscle, the same can happen to your nerves! It often occurs between the 3rd and 4th toes, though can occur in between the 2nd and 3rd toes , and may be a palpable round mass.
The cause of a neuroma is often repetitive compression of the nerve which may occur from:
Does it feel like you’ve been walking around on an uncomfortable small stone beneath your foot for some time now? Have you been feeling pain at the forefoot that seems unusual? And that while Google tells you this pain should be located beneath the big toe joint or at one of the other toes along the ball of your foot, you’re actually feeling it up from there, through the long bones of the foot? Perhaps around your 3rd and 4th long toe bones? And maybe instead of the usual pain, redness and swelling, the pain and discomfort comes with a twinge every so often that may tingle or feel numb?
If this sounds familiar then you, my friend, may have a Morton’s Neuroma.
What is a Morton’s Neuroma?
A neuroma describes a thickened or inflamed nerve in a space between the toes (interdigital space). Just like rubbing and irritating a muscle, the same can happen to your nerves! It often occurs between the 3rd and 4th toes, though can occur in between the 2nd and 3rd toes , and may be a palpable round mass.
The cause of a neuroma is often repetitive compression of the nerve which may occur from: