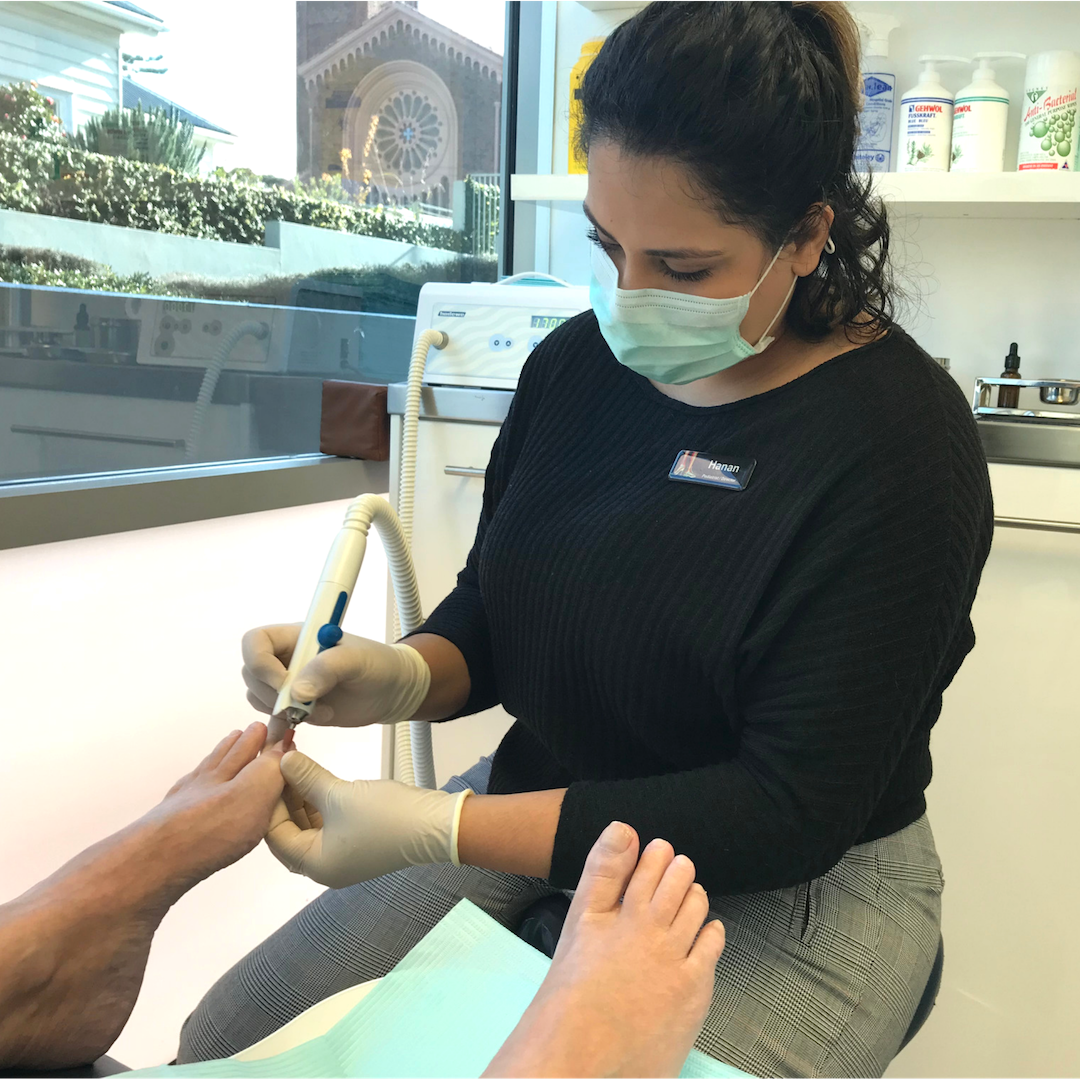
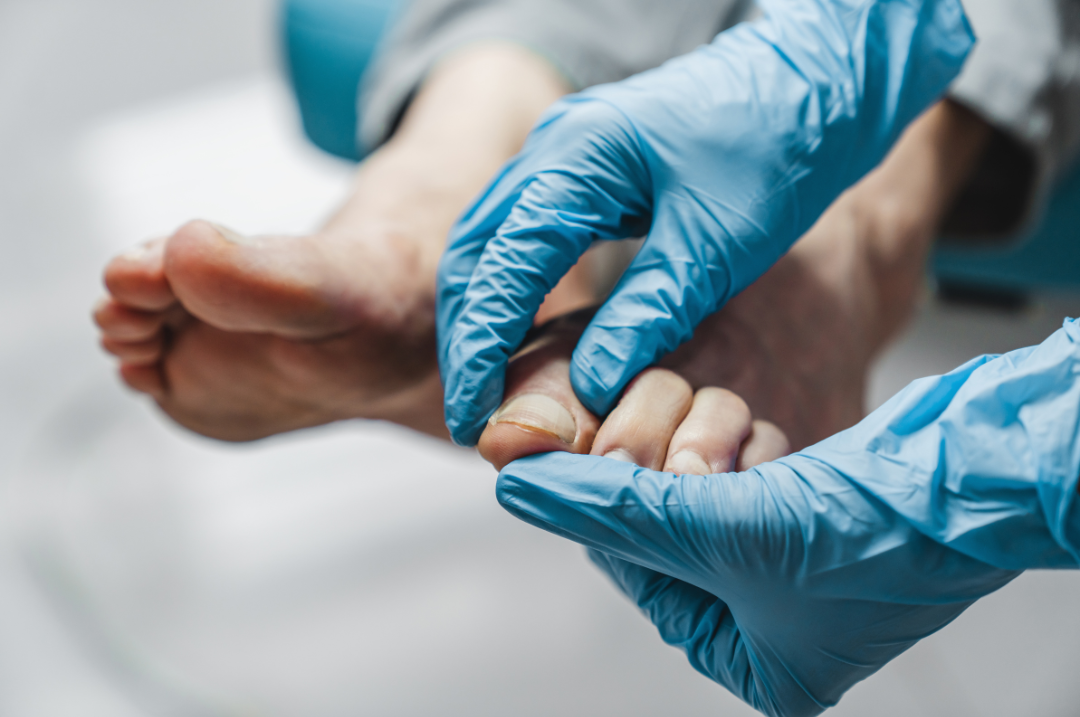
What causes Charcot foot?
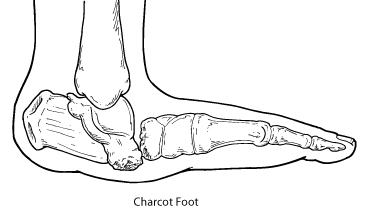 Charcot foot is caused by the weakening of the bones and joints in people that have significant damage to their nerves, known as neuropathy. Neuropathy is a common complication of diabetes, though can also be caused by other conditions such as alcoholism.
As the bones weaken, they are vulnerable to fracturing and dislocating. Because neuropathy impacts a person’s ability to feel and detect pain, they may continue to walk and cause subsequent fractures and damage. Because no impact trauma (like a fall or a hit) has occurred, they won’t realise that the risk of a fracture is present. Ultimately, this leads to the collapse of the joints in the feet.
A bone fracture, break, or sprain that is not effectively managed can also create the right conditions that trigger a chain of events that lead to Charcot foot.
Charcot foot is caused by the weakening of the bones and joints in people that have significant damage to their nerves, known as neuropathy. Neuropathy is a common complication of diabetes, though can also be caused by other conditions such as alcoholism.
As the bones weaken, they are vulnerable to fracturing and dislocating. Because neuropathy impacts a person’s ability to feel and detect pain, they may continue to walk and cause subsequent fractures and damage. Because no impact trauma (like a fall or a hit) has occurred, they won’t realise that the risk of a fracture is present. Ultimately, this leads to the collapse of the joints in the feet.
A bone fracture, break, or sprain that is not effectively managed can also create the right conditions that trigger a chain of events that lead to Charcot foot.
What are the symptoms?
Symptoms begin at the foot and ankle and may include:- Redness
- Warmth
- Swelling
- Pain (where it is able to be felt)
How is Charcot foot treated?
Because the effects of Charcot foot can be limb-threatening, effective management must be undertaken. Each case is assessed independently and takes into consideration the extent of the changes, your risk and current symptoms. Treatment may include:- Off-loading and immobilising the foot and ankle to allow the adequate repair of the bones and prevent further collapse. This may require a splint, cast, boot, brace or even wheelchair.
- Orthotics, braces and footwear can be used after the bones have healed to reduce the risk of recurrence, help with movement (especially if the foot position has changed) and reduce the risk of ulcer development