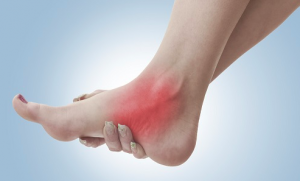
What is tarsal tunnel syndrome?
Tarsal tunnel syndrome (TTS) describes the compression of and damage to the tibial nerve as it passes through the tarsal tunnel and beneath the connective tissue sheath (flexor retinaculum).What causes tarsal tunnel syndrome?
While some cases of tarsal tunnel syndrome have can have no attributed cause, tibial nerve compression can be caused by:- Repetitive impact activities such as running
- Trauma/injury to the ankle
- Abnormal foot alignment and position, such as flat feet (pronation)
- Inflammation of structures within the tarsal tunnel, including abnormal growths or cysts
- Tarsal coalition
- Inflammation and compression from systemic conditions such as arthritis or diabetes
What are the symptoms?
- Burning pain
- Shooting pain
- Tingling
- Numbness
- Pins and needles
How is it treated?
While initially rest, ice and anti-inflammatories may help reduce painful symptoms, treating tarsal tunnel syndrome is centred around treating the particular cause of the nerve compression where it is known or deduced. Your Podiatrist will run through a thorough exam to assess the function and characteristics of your feet and legs. Management may include:- Custom-designed orthotics to open the tarsal tunnel, relieve pressure from the tibial nerve, and correct any biomechanical abnormalities that may be contributing to the pain and onset of symptoms
- Activity modification to reduce the stress on inflamed tendons or other structures that are located within the tarsal tunnel
- Assessing footwear to ensure it is keeping your foot in a good and stable position to not aggravate symptoms
- Physical therapy (stretching and strengthening) to rehabilitate the foot and its musculature
- Gait retraining
- Bracing – Patients with flatfoot or those with severe symptoms and nerve damage may be fitted with a brace to reduce the amount of pressure on the foot.
- Immobilization – Restricting movement of the foot by wearing a cast is sometimes necessary to enable the nerve and surrounding tissue to heal
- Oral medications – Nonsteroidal anti-inflammatory drugs such as ibuprofen, help reduce the pain and inflammation.