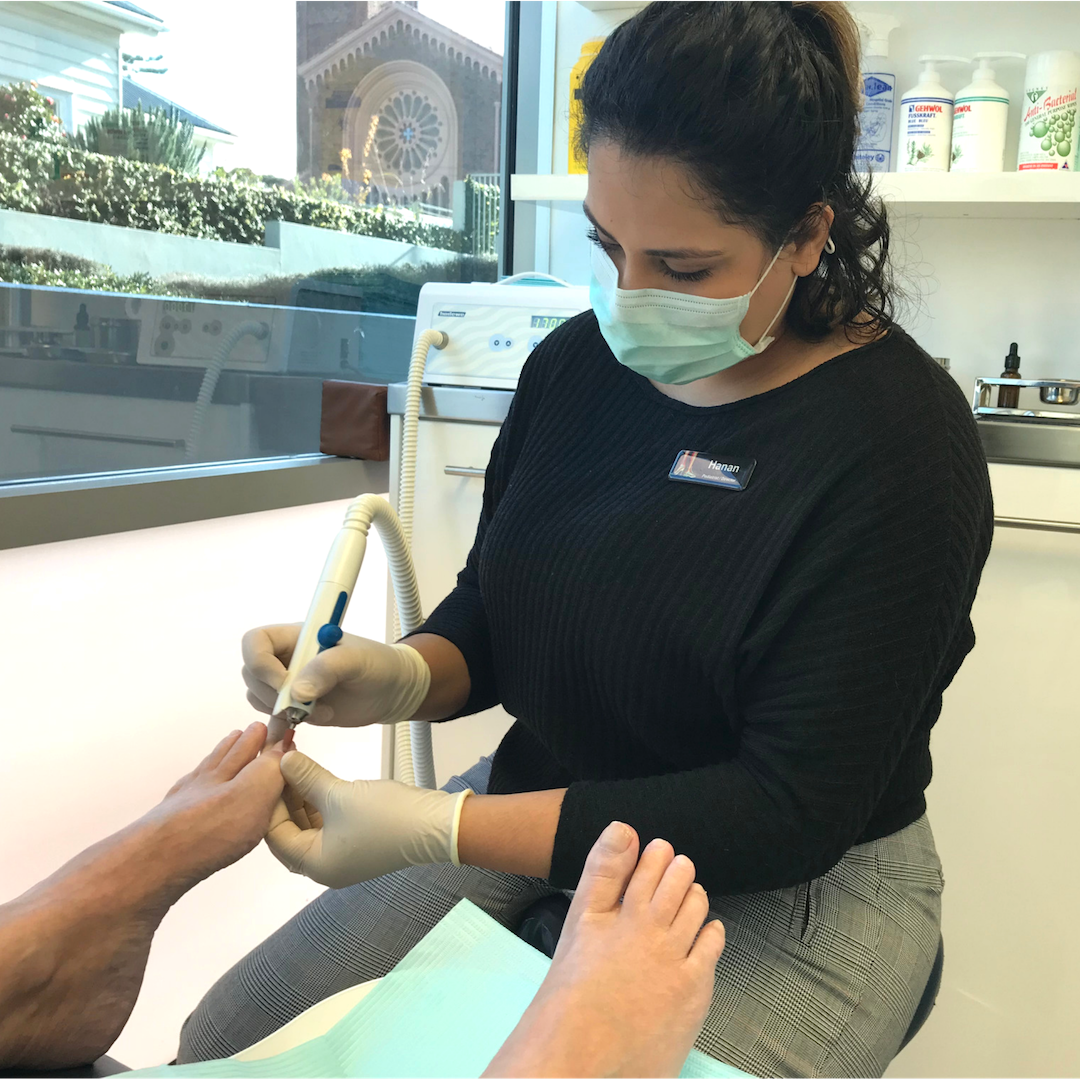
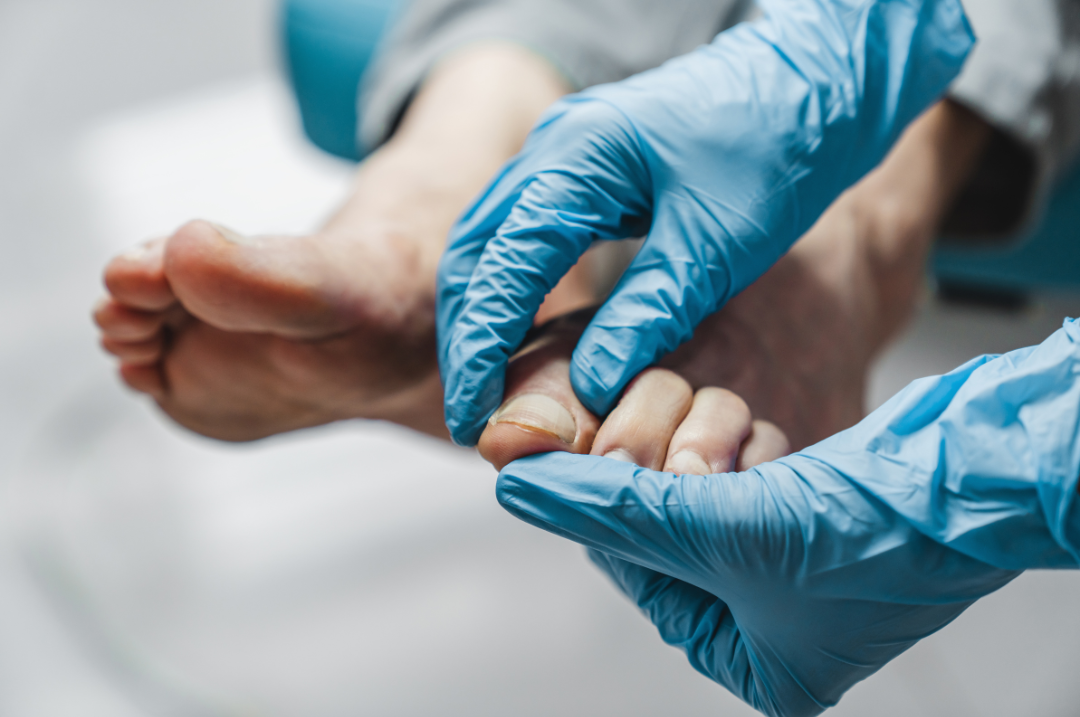
Essential terminology: Your ‘plantar fascia’ is a thick band of connective tissue that attaches to your heel and then spans your foot like a fan to connect to all five toes. You have connective tissues all around your body. In fact, connective tissue is one of the four main tissue types. It serves to connect, stabilise and enclose musculature and structures throughout the human body. Then plantar fascia helps maintain the shape of the foot by supporting the bones, joints and muscles, thereby helping to maintain the shape of your arch.
What is Plantar Fasciitis?
Plantar Fasciitis describes the damage and subsequent inflammation to your plantar fascia (see above). When the fascia is overloaded with pressure, strained or directly damaged, it becomes inflamed. It is this inflammation that causes the painful symptoms that is known as plantar fasciitis.
What causes Plantar Fasciitis?
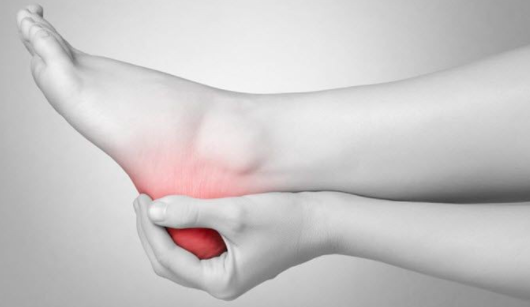
As the plantar fascia spans the arch, it is stretched every time we take a step. The body is well used to this and our normal daily walking and activities. However, if we overuse, overload or generally strain the fascia past the point that it can handle, it will develop microtears through its fibres, causing damage and inflammation.
The plantar fascia can become damaged from a variety of causes, including:
- A sudden increase in physical activity or the intensity of activity
- Particular activities that strain the arch such as climbing stairs
- Wearing shoes that don’t support the arch and fascia – especially if you’re used to wearing supportive footwear regularly
- Your foot type or foot biomechanics that put a greater load or force through the fascia (like a flatter foot)
- Trauma to the insertion of the fascia at the heel, such as jumping down from a high surface
- Faulty training technique
- Increased weight
It is important to not only look at the symptoms but the cause so that the fascia doesn’t keep getting damaged in the future. This happens when the cause isn’t a one-off activity but associated with the biomechanics of your feet, which is often a primary cause of plantar fasciitis.
What are the symptoms?
Common symptoms of plantar fasciitis include:
- Pain at the bottom of the heel that may radiate into the arch
- Swelling
- Pain on standing first thing in the morning
- Pain on standing after rest
- Pain may come and go, or be constantly present. Often pain can ease a few minutes after you start walking around
- Pain can range from a mild discomfort to an intense stabbing pain
Symptoms can come and go over months or even years, without the problem being resolved. Because the damage to the fascia can worsen, this condition must be effectively managed to prevent a partial tear, or even the complete rupture, of the plantar fascia.
Care must also be taken as the symptoms of other conditions may also closely match the symptoms of plantar fasciitis. A good example of this is Abductor Hallucis Tendinopathy, where the Abductor Hallucis muscle shares an insertion at the base of the heel with the plantar fascia.
How is it treated?

The first step to treatment is getting a complete picture of what is happening with your feet and what the cause is, especially as there are often multiple contributing causes. From there, your Podiatrist will create a comprehensive treatment plan for you that takes into consideration your daily activities, lifestyle and goals. Initially, the focus of the treatment plan will be to reduce your current symptoms and get you out of pain, while long-term your treatment plan will work to prevent this from happening again. Once you’ve had plantar fasciitis, you’re more likely to damage your fascia again, so this must be a primary focus.
Depending on the severity of your symptoms, your treatment may include:
- Orthotic shoe inserts – these will support the arch and reduce strain and tension on the plantar fascia so it can begin to heal as opposed to being constantly stretched during walking. Custom orthotics can also correct any faulty foot biomechanics you may have that contributed to this condition developing
- Stretching – once the initial pain and inflammation settle, and you are able to handle gentle stretching, stretching the fascia can help reduce and prevent the onset of painful symptoms. Because other tight muscles in the feet and legs can pull on the heel and therefore the fascia, stretching will also focus on other tight muscle groups too
- Strengthening – working to strengthen the muscles of the feet and legs can improve your overall foot and leg function, thereby reducing the risk of injury. Strengthening exercises will be prescribed on a case-by-case basis after reviewing the results of your assessment.
- Footwear – your regular footwear will be checked and discussed to make sure it’s helping your recovery and not hindering you
- Strapping – strapping can reduce painful symptoms by keeping your foot in a position that relieves strain and pressure from the plantar fascia
- PRICE – protection, rest, ice, compression and elevation may be initially used to reduce pain and swelling
Depending on your symptoms and circumstances, various other treatment modalities may be recommended for your recovery, such as splints and pads.
Will the pain come back?
The answer to this is truly dependant on you. Just like you can break your leg or sprain your ankle twice, you can definitely suffer from plantar fasciitis again. They key is to have the right preventative measures in place to reduce the risk of this happening again. By knowing about the condition and its causes, you can also make the best decisions for your feet. Make sure you talk through any questions you have with your Podiatrist and understand how to best protect and look after your feet.